How to Build a Patient Recall System That Boosts Revenue
Have you ever wondered why a patient recall system matters so much for a successful medical practice? If you’re tired of no-shows, unpredictable revenue, and patients falling through the cracks, you’re in the right place. By the end of this guide, you’ll know how to build a recall process that boosts revenue, improves outcomes, and keeps your schedule steady — without burning out your team.

Key Takeaways:
- Patient recall systems reduce no-shows
- Boosts preventive and chronic care revenue
- Supports quality programs like MIPS and HEDIS
- Automation saves staff time and increases consistency
- Builds patient loyalty and trust
- Protects continuity of care
- Supports higher payer incentives
- Critical for practice sustainability
Table of Contents
How Can Patient Recalls Protect Gaps in Care?
Here’s a quick reality check: patients forget things. They get told so many things in one appointment that most of it goes straight out the window by the time they get home. Without a patient recall process, you risk patients falling through the cracks, missing their follow-ups, or losing track of their chronic care plans.
That’s what the medical world calls “lost to follow-up.” And it’s expensive.
By running a recall system, you close those gaps and keep chronic conditions from getting out of hand. Whether you’re focusing on preventive care revenue (like annual physicals) or managing a patient’s diabetes, you need them to come back. That’s where patient recall strategies shine. They safeguard continuity of care in healthcare, protect patients, and protect your bottom line.
Definition: A patient recall system is a structured process that proactively contacts patients to remind or schedule needed follow-up visits.
When your staff uses technology to schedule, remind, and confirm appointments, you dramatically reduce the risk of no-shows and treatment plan derailments. This reduces no-shows in your medical practice while protecting revenue.
How Can a Patient Recall Process Stabilize Visits?
You bet they can. A medical practice patient recall process is the secret sauce to stabilizing your appointment book.
Picture this: you only rely on new patients to fill your schedule. That means your revenue is a roller coaster. Some weeks, you’re slammed. Other weeks, the phones barely ring.
Instead, if you build a workflow that recalls patients for routine things — like three-month blood pressure checks, yearly labs, or follow-up imaging — you can count on a steady flow of appointments. That means a steadier income stream and easier staffing decisions.
Here’s a quick breakdown to see how it plays out:
| Patient Recall Benefit | Impact on Practice |
|---|---|
| Regular follow-up visits | Steady appointment volume |
| Proactive chronic care | Better patient outcomes |
| Consistent schedule | Easier to forecast staff needs |
| Repeat billing opportunities | Higher, predictable revenue |
Summer months tend to be slower for many practices, for example, while back-to-school season often sees a rush. With a recall plan, you can even out those peaks and valleys and stop worrying about how to pay your staff next month.
How Do Patient Recalls Increase Billing Revenue?

Let’s talk money — because your practice is a business too.
When patients come in for a recall appointment, they rarely leave without something else being done. Maybe you draw blood for labs, maybe you do an EKG, or maybe you order an X-ray. Those services are billable.
That means each patient recall is more than one visit — it can open the door to other billable procedures. Even small charges add up.
Here’s a relatable scenario:
A patient comes in for a routine hypertension follow-up. You check their vitals, renew their medication, and notice they’re overdue for cholesterol labs. Boom — you bill the E/M code for the visit plus the lab draw. Those little additions keep the revenue flowing and support practice sustainability.
So think of a patient recall workflow as a way to maximize billing opportunities. It keeps the doors open, the lights on, and your patients healthier, supporting practice sustainability.
How Do Patient Recalls Improve Quality Metrics?
If you’re part of a value-based care program — like MIPS or HEDIS — you know how important it is to track quality measures. Payers and insurance plans look closely at how well you follow patients and manage their chronic conditions.
Learn more about MIPS from the official CMS program overview on Medicare’s MIPS program.
A robust patient recall system helps you hit those targets. You’ll get better scores, qualify for incentive payments, and even negotiate better rates with payers. That means more money in your pocket and less risk of penalties for falling short.
Plus, when you can document consistent recalls, you’re showing insurers you take continuity of care in healthcare seriously. That builds trust and gives you a competitive edge.
Takeaway: A consistent patient recall process is your ticket to higher incentives, fewer penalties, and stronger payer relationships.
How to Set Up a Patient Recall System Step by Step
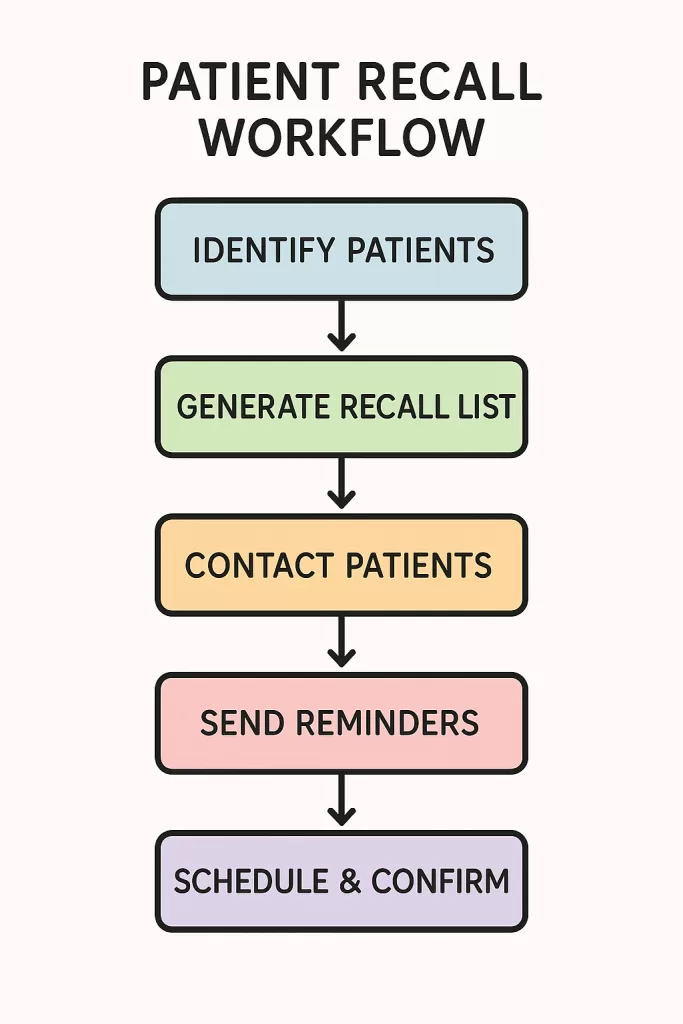
So you’re convinced by now that a patient recall system is mission critical — but how do you build one that actually works? Let’s break this down without making your head spin.
A recall system is really a workflow. It starts with identifying patients who need to come back, then moves into communicating with them, scheduling them, and tracking that it actually happened. It might sound intimidating, but you can absolutely design a recall system even in a small practice with minimal staff.
The first step is to define who needs to be recalled. Think about chronic care management patients, annual preventive visits, medication reviews, lab rechecks, follow-up imaging — anything that requires a scheduled recheck should go on the list.
Next, put a timeline around it. If the patient’s due for a yearly physical, you want your recall to kick in maybe 30–60 days before they’re due. For shorter follow-ups, like a two-week post-procedure check, the recall notice needs to go out right after their initial visit so it’s on their radar.
Definition: Patient recall workflow = a repeatable process that identifies patients needing follow-up, reminds them, reschedules them, and verifies completion.
The simpler you make it, the better. That’s where technology comes in, and trust me, you don’t want to manually call every single patient from a spreadsheet.
Which Tools Automate a Patient Recall System?

Let’s be honest: if you’re trying to do this with sticky notes, you’re going to burn out fast. That’s why you should lean into technology.
Most modern EHR systems include a patient recall process tool built right in. They can automatically track which patients are due, send a text or email reminder, and even tee up your staff to make a phone call if the patient doesn’t respond.
If your EHR doesn’t have a solid recall function, there are dedicated third-party tools that integrate with your practice software. They’re built to handle exactly this kind of thing, including sending voice calls, two-way texts, or portal messages.
Here’s a look at what technology can do:
| Recall Tool | How It Helps |
|---|---|
| Automated texting | Fast, low-effort reminders patients actually see |
| Email notifications | Reaches patients who check email more than voicemail |
| Portal messaging | Keeps everything documented securely |
| Phone call automation | For patients who don’t do tech or need a personal touch |
The best part? You don’t have to do all the follow-up manually. Your staff will thank you, your patients will thank you, and your schedule will run smoother.
How Should You Train Staff for Recalls?
Even with fancy automation, you’ll need your staff to run a patient recall process. If no one takes ownership of the workflow, it will fall apart. Guaranteed.
First, set clear roles. Who is responsible for checking overdue lists each week? Who sends out recall messages? Who follows up if there’s no response?
Train everyone on why recalls matter, so they’ll be motivated to own the how. Show them how it reduces no-shows in medical practice, stabilizes revenue, and improves patient compliance.
It’s also smart to build simple scripts. If a patient says, “Why do I need to come back?”, your staff should have a quick explanation ready. Something like:
“Our doctor wants to see you to monitor your progress and prevent bigger problems down the road. It’s covered by insurance and helps keep your treatment on track.”
Short, confident, and helpful. That’s how you get patients on board.
How to Track and Measure Recall Performance?
You can’t just set it and forget it. A successful patient recall system needs measuring and tweaking.
Check weekly how many patients were contacted, how many responded, and how many showed up. If your no-show rate stays high, dig into why. Are the messages clear? Do they go out at the right time? Are you giving patients enough appointment options?
A simple table in your practice dashboard can help you stay on top of things:
| Metric | Goal |
|---|---|
| Recall response rate | Over 80% |
| Completed visits | 90% of scheduled patients |
| No-show rate | Under 5% |
Pro tip: Share these numbers with your team each month to show progress and keep everyone motivated.
How Patient Recalls Support Long-Term Sustainability
When you put all these pieces together, you get more than just a smoother schedule — you build practice sustainability.
A consistent recall process protects your cash flow, boosts patient trust, and supports chronic care management. Patients stay healthier, and you don’t waste precious resources trying to chase down missed appointments or handle last-minute cancellations.
Remember, the best patient recall system is proactive. You reach out before things slip through the cracks. That means fewer lost visits, better care, and a steady revenue stream you can count on month after month.
Takeaway: A well-run recall process is the backbone of a sustainable, patient-focused medical practice.
What Roadblocks Should You Watch Out for in Patient Recalls?

Even the best patient recall system will hit a few speed bumps, so let’s be real about them. One of the most common obstacles is patient confusion. They often don’t understand why they need to come back, especially if they “feel fine.” It’s your job to help them see that follow-ups are about staying fine, not just treating problems when they happen.
Another classic barrier is staff burnout. If your recall workflow is clunky or overloaded, your team will quickly see it as “extra work” instead of a practice-sustaining strategy. That’s why training, ownership, and easy-to-use tools matter so much.
And let’s not ignore tech headaches. Maybe your EHR doesn’t sync, or reminders aren’t going out on time. If you see tech glitches, fix them fast. Patients won’t be patient about their reminders — pun intended!
Quick tip: Run a monthly test of your recall system. Pretend you’re the patient and make sure the reminders actually land. Nothing kills a great plan faster than a broken notification system.
Why Does Recall Compliance Matter to Payers?
Here’s where it gets serious. Payers (insurance companies) watch your recall rates closely. If you claim you give continuity of care in healthcare, they want proof. That means you must document every outreach attempt, every patient response, and every scheduled visit.
When you show data, you build trust and protect yourself from audits. Good recall compliance also supports MIPS or HEDIS quality measures, which can mean bonus payments and stronger contracts.
Let’s look at how this might play out:
| Payer Requirement | How Patient Recalls Help |
|---|---|
| Chronic condition monitoring | Documents follow-up for diabetes, hypertension, asthma, etc. |
| Preventive care revenue goals | Proves annual screenings are offered and completed |
| No-show rate reporting | Shows active outreach to reschedule patients |
So if you ever get pushback about your incentive payments, you’ll have a rock-solid defense: a documented patient recall process that proves you did everything you could to keep your patients on track.
What Advanced Recall Strategies Can You Use?
If you want to take your medical practice patient recalls to the next level, borrow a few tricks from the big hospital systems.
First, use segmentation. That means putting patients into groups — chronic care, preventive, post-op, or wellness visits — and tailoring your messages to each group. A diabetic patient should not get the same “We miss you!” text as a healthy teen due for a sports physical. Speak their language.
Second, look for opportunities to combine appointments. Let’s say a patient is due for a blood draw and a physical. Don’t make them come twice. Bundle those visits, which saves them time and fills your schedule efficiently.
Third, use patient feedback to fine-tune your workflow. After each recall, send a simple survey. Did they understand the reminder? Was it easy to book? You’ll get gold nuggets of insight that you can put right back into your process.
Definition: Patient segmentation is the practice of grouping patients by their health needs or visit reasons to deliver customized outreach.
If you apply these advanced tactics, you’ll see even stronger results — more loyal patients, higher revenue, and fewer headaches for your team.
How Do Patient Recalls Improve Patient Loyalty?

People want to feel cared for, not just processed. When you run a reliable patient recall system, patients notice. They see you are proactive about their health, that you remember them, and that you’re invested in keeping them well.
This personal touch is what keeps patients coming back — and not wandering off to the shiny new practice down the street. When a patient feels like they matter, they will stay with you, follow your advice, and even tell their friends.
It’s also about trust. A recall system shows you take their treatment plans seriously and value their time. That creates loyalty, plain and simple.
Takeaway: Patient recalls aren’t just about appointments — they’re about building trust and long-term relationships.
What’s the Big Picture for Patient Recalls?
Absolutely. Think of patient recalls as the backbone of a modern, sustainable practice. They protect revenue, boost care quality, satisfy payers, and keep patients engaged. If you want a practice that’s future-proof, this is non-negotiable.
Here’s a snapshot of how it all ties together:
| Benefit of a Patient Recall System | Why It Matters |
|---|---|
| Revenue stability | Predictable income, fewer surprises |
| Better patient outcomes | More consistent treatment and monitoring |
| Staff efficiency | Less last-minute scrambling and no-shows |
| Higher payer trust | Supports contracts and incentives |
It’s a revenue machine, a quality driver, a loyalty builder, and a schedule stabilizer all rolled into one. If that’s not worth investing in, I don’t know what is.
How Can You Measure the ROI of Your Patient Recall System?
OK, you’ve set up your patient recall process — but how do you know it’s working? Let’s talk about measuring return on investment (ROI).
First, track the numbers that matter. How many patients responded to your recalls? How many showed up? What revenue did those visits generate? The easiest way to calculate ROI is to compare the money coming in from follow-up visits to the costs of running your recall program — including staff time, software, and outreach expenses.
Here’s a simple table to help you think through it:
| Metric | How to Measure |
|---|---|
| Recall outreach cost | Staff hours + software fees + other expenses |
| Revenue from follow-up visits | Total collected from billed services linked to recalls |
| Net profit | Revenue from recalls minus outreach cost |
| Response rate | Percentage of patients who book after a recall contact |
For most practices, a well-run patient recall workflow pays for itself many times over. Even one or two extra visits per day can add thousands of dollars per month — money you would otherwise leave on the table.
What Success Stories Can Inspire You?
Plenty of practices have transformed their operations with a solid patient recall system.
For example, a primary care clinic that focused on annual wellness visits increased its preventive care revenue by 30% within six months. Why? Because patients were reminded, scheduled, and showed up for the exams that were covered 100% by insurance.
Another small endocrinology practice cut its no-show rate from 20% to under 5% after automating recall messages through text reminders. They boosted their follow-up rates, improved chronic care management, and even scored higher on their quality incentive payments because patients stuck with their plans.
These aren’t giant hospital systems with huge budgets. These are regular practices using a simple, steady patient recall strategy to boost outcomes and keep revenue stable.
Takeaway: Even the smallest practice can see big results with a consistent patient recall process.
What Is a Good Checklist for Running Recalls?
Ready to build your own? Here’s a simple, no-fluff checklist to get you going.
First, define who should be recalled. That might be annual wellness, medication monitoring, lab checks, or post-op patients.
Next, pick a timeline. Remind them early enough so they can get on your schedule — but not so early they forget about it.
Then, build your messages. Keep them short, friendly, and clear. Let patients know why the follow-up matters.
After that, assign staff roles. Someone should monitor the system, send messages, and confirm appointments.
Finally, track your results. Measure recall response rates, revenue, and no-show patterns. Adjust and improve over time.
Here’s a clean summary you can copy:
| Step | Action |
|---|---|
| Identify patients | Define which visits need a recall process |
| Choose timing | Set reminder dates based on visit frequency |
| Craft messages | Friendly, helpful, and easy to understand |
| Train and assign staff | Make sure everyone knows their role |
| Monitor results | Check performance, measure, and improve |
A patient recall system only works if you manage it, measure it, and keep fine-tuning it.
Why Should You Care About Patient Follow-Up Strategies?
Because follow-up is where the magic happens. Patients leave your office full of advice and action plans, but their motivation fades fast. A patient recall system is the nudge they need to stay on track.
Whether you focus on reducing no-shows in medical practice, improving patient compliance, or just keeping the doors open with steady revenue, recall systems are the key.
They make your practice proactive, building trust and stronger follow-through.
Definition: Patient follow-up strategies are systematic actions that encourage patients to complete their care plans after an initial visit.
When patients feel you’re invested in their health, they return the favor with loyalty. And that is priceless.
What Should Be in Your Patient Recall SOP?
If you’re ready to lock this down, you’ll want to build a standard operating procedure (SOP) for your patient recall system. Think of this like your practice’s playbook. It tells your team what to do, so there’s no confusion, no guessing, and no missing patients.
Your SOP should include:
1. Who is responsible — list staff members or roles in charge of recalls.
2. Which patients get recalled — spell out the criteria, such as annual wellness, chronic condition follow-ups, or lab rechecks.
3. When to send reminders — define the timing clearly (e.g., 30 days before due, 7 days before, 24 hours before).
4. How to send reminders — text, email, phone calls, or a combo? Outline exactly how you want it done.
5. How to document — note every attempt in the EHR so you have proof for payers, risk management, and your own peace of mind.
Here’s a simple table you can adapt:
| SOP Section | What to Include |
|---|---|
| Responsibility | Assign staff or positions |
| Patient criteria | Define who should be recalled |
| Timing | Schedule for sending messages |
| Communication methods | Text, email, portal, phone |
| Documentation | Where and how to track recall attempts |
For a broader look at developing clear, practical office policies, see this guide on creating and maintaining medical practice policies and procedures.
What Scripts Can Staff Use for Patient Recalls?
If your staff feels awkward about calling patients back, make their lives easier with a simple script. You don’t want robotic conversations, but you do want consistency.
Here’s a flexible sample:
“Hi, this is [Name] from [Your Practice]. I’m calling to help you stay on track with your [condition/preventive visit]. Dr. [Doctor] would like to see you to [reason — for example, check your blood pressure or review labs]. We can get you scheduled this week if that works for you. What day would be best?”
Keep it warm, confident, and focused on value for the patient. They should feel like you’re helping them — not bugging them.
If patients push back, staff should have a quick reason ready:
“This visit is important to help you stay healthy and catch any problems early. It’s usually covered 100% by your insurance.”
A good recall conversation is about reassurance. The goal is to build trust, not sound like a collections call.
Which Reporting Templates Track Recalls Best?
You’ll also want to track, track, track. A simple reporting template can be a lifesaver. At a minimum, you should review:
- The number of recalls sent
- Response rates
- Completed appointments
- No-show rates
- Revenue tied to recall visits
Here’s a table you can copy and tweak:
| Metric | This Month | Goal |
|---|---|---|
| Recalls sent | 500 | 1000 |
| Response rate | 60% | 80% |
| Completed appointments | 275 | 400 |
| No-show rate | 12% | Under 5% |
| Revenue from recall visits | $15,000 | $30,000 |
Your monthly huddle should include reviewing these numbers. If you see your goals slipping, brainstorm why — maybe the timing is off, maybe patients don’t like your messages, maybe your staff isn’t following the SOP. That’s where a consistent review process pays off.
Why Is Documentation Vital for Patient Recalls?
Payers, auditors, risk managers, and even patients want evidence. If you claim you’re running a patient recall system, you need to prove it.
That means tracking every single contact. Whether you called, texted, or sent a portal message, you must log it. This protects you against claims of negligence if a patient misses a needed visit. It also supports your quality metrics and reimbursement incentives.
In other words, documentation is your shield.
Takeaway: If you didn’t document it, it didn’t happen — at least in the eyes of payers and auditors.
So, yes, a patient recall strategy is about patient care. But it’s also about protecting your practice.
How Should You Recall High-Risk Patients?
Your patient recall system isn’t one-size-fits-all — especially when you deal with high-risk patients. These are folks with complex chronic conditions, multiple medications, or a history of missing visits. They need a stronger safety net.
For these patients, don’t rely on a single reminder. Consider layering your approach. Send a text, then follow up with a call, and if they still don’t schedule, have a staff member personally reach out. High-risk patients benefit from that personal touch, and it often keeps them from falling through the cracks.
Here’s a helpful way to think about it:
| Patient Type | Recommended Recall |
|---|---|
| Routine preventive | Text or email |
| Chronic stable | Text plus occasional call |
| High-risk/chronic fragile | Personal call, multiple reminders, confirm scheduling |
These high-risk patients might also need a family member or caregiver looped in. Make sure you have the right permission to speak with a spouse, child, or case manager if it helps keep the patient engaged.
Proactive outreach saves lives — and protects your practice from gaps in care.
How Should Pediatric Patient Recalls Work?
Pediatrics brings its own twist to the patient recall process. Kids grow fast, and they have vaccine schedules, sports physicals, developmental screenings, and all those milestone visits.
Parents are usually on board with recalls if you make them easy and friendly. Instead of a generic “time for a checkup” message, highlight what the visit includes — like shots, growth tracking, or school forms. Parents want to know you’re keeping their child’s health on track, not just selling them another appointment.
For example:
“Hi! [Child’s name] is due for their wellness visit. We’ll check their growth, answer any school health questions, and update vaccines. Call us to get a time that works for you!”
That feels supportive and parent-centered, instead of cold or transactional.
Pediatric practices should also coordinate recalls with public health vaccine campaigns to help protect your youngest patients and build community trust.
How to Recall Behavioral Health Patients?
Behavioral health needs a gentle, consistent, and nonjudgmental approach. Patients dealing with depression, anxiety, or substance use disorders may avoid appointments because of stigma or fear.
That’s why your recall messages should be encouraging and kind. Avoid language that feels demanding or controlling. Instead, highlight support and continuity. For example:
“We’re here to help you stay on track and support your wellness plan. Let’s get your next session scheduled — you matter to us.”
It’s also helpful to offer flexible options — telehealth, phone check-ins, or shorter in-person visits — to make follow-ups feel less overwhelming.
Behavioral health recalls can literally change lives, so make them a priority.
How to Recall Geriatric Patients Effectively?
Older patients deserve a patient recall process tailored to their needs. They might have trouble getting rides, memory issues, or many conditions at once.
Always offer extra time in your messaging and call attempts. If they don’t respond to a text, have someone follow up with a call. And be prepared to speak slowly, repeat details, or talk to a caregiver.
It can also help to confirm whether they need transportation resources or assistance getting to your office. Many local community programs offer rides for seniors — you can include that info in your recall reminder.
“Your next appointment helps us monitor your health and keep you strong. If you need a ride, let us know and we can help find resources.”
Older patients appreciate this thoughtful approach, and it strengthens their trust in your practice.
Why Should You Tailor Recall Strategies to Patients?
Because cookie-cutter reminders aren’t enough. Different patients have different needs, risks, and barriers. When you adapt your patient recall system to these special cases, you show your practice truly cares about the person — not just the chart.
This builds loyalty, improves outcomes, and protects your revenue at the same time. Plus, you’ll sleep better knowing no one fell through the cracks because you customized your process.
Takeaway: Personalized recalls are the heart of a people-first medical practice.
Patient Recall System Frequently Asked Questions
What is a patient recall system in a medical practice?
A patient recall system is a step-by-step process that helps you remind patients about follow-up visits, checkups, or screenings. It uses tools like texts, emails, or calls to get them scheduled on time. This protects continuity of care and helps your practice’s revenue.
How can a patient recall process reduce no-shows?
Patient recalls help cut no-shows by sending reminders and clear instructions, so patients remember their visits. Combining automated texts with personal calls makes them less likely to forget or skip needed follow-ups, which protects your revenue and care quality.
Why are recalls important for chronic care management?
Recalls are key for chronic care because they keep patients on track with treatment. Regular reminders help them come back for monitoring, labs, or medication changes. This stops conditions from getting worse and supports better health, while also meeting payer and quality rules.
Can small practices handle patient recalls effectively?
Yes! Even small practices can run a good patient recall system using simple EHR tools, free text messages, or low-cost software. The key is to build a repeatable plan, give people clear jobs, and track results so no patients slip through the cracks.
How do patient recalls help improve practice revenue?
Patient recalls boost revenue by getting patients to book follow-ups, which often include billable labs or imaging. This steady flow of appointments keeps income stable and helps avoid gaps when patients miss care or don’t reschedule.
Final Thoughts on Building a Strong Patient Recall Process
We’ve covered a lot — from why a patient recall system matters, to how to build one, train staff, document everything, and even handle special cases like kids, seniors, and behavioral health patients.
By now, you can see patient recalls aren’t just an afterthought. They’re a strong strategy that keeps your revenue steady, improves patient results, protects you from risk, and supports a healthy practice.
When you remind patients ahead of time, you protect them from falling through the cracks. You lower no-shows, keep plans on track, and build loyalty that lasts. Whether you’re a solo family doctor, a pediatric group, or a specialist, a patient recall workflow is like guardrails for your practice — it keeps things safe and steady.
If you want to take your recall process to the next level, remember these essentials:
- Personalize your messages
- Train and empower your team
- Automate where you can
- Track your results
- Adjust and improve continuously
Every practice is different, but the principles stay the same. Stay consistent. Stay proactive. And stay focused on why you’re doing this in the first place: to help patients live healthier, better, more connected lives.
