Insurance Payment Retractions In Medical Billing
Everything can look normal in your revenue cycle—claims are being paid, cash is coming in, and posting is moving along—until a negative adjustment shows up on an ERA or EOB.
That’s usually your first sign of a takeback.

Insurance takebacks, also called retractions, are one of the more disruptive issues in billing operations because they reverse revenue you’ve already recorded. If they’re not handled correctly, they create confusion in reconciliation, delay financial reporting, and in some cases, introduce compliance and collections risk.
The challenge is not just understanding that a takeback happened—it’s knowing how to respond quickly and accurately before it turns into a larger operational problem.
What an Insurance Takeback Actually Means
A takeback occurs when an insurance company determines that a payment they previously issued was incorrect and needs to be reversed.
This reversal can appear in different ways. Sometimes it’s clearly tied to a specific claim with a remark code explaining the adjustment. Other times, it shows up as a negative amount without clear attribution, which is where the real difficulty begins.
From an operational standpoint, a takeback is not just an accounting adjustment. It represents a change in claim status that requires action—either correcting the original claim, returning funds, or disputing the payer’s decision.
Why Takebacks Create Operational Confusion
The biggest issue with takebacks is inconsistency.
Payers do not handle retractions the same way. Some provide detailed explanations tied to specific claims. Others provide minimal information, leaving your team to investigate where the adjustment originated.
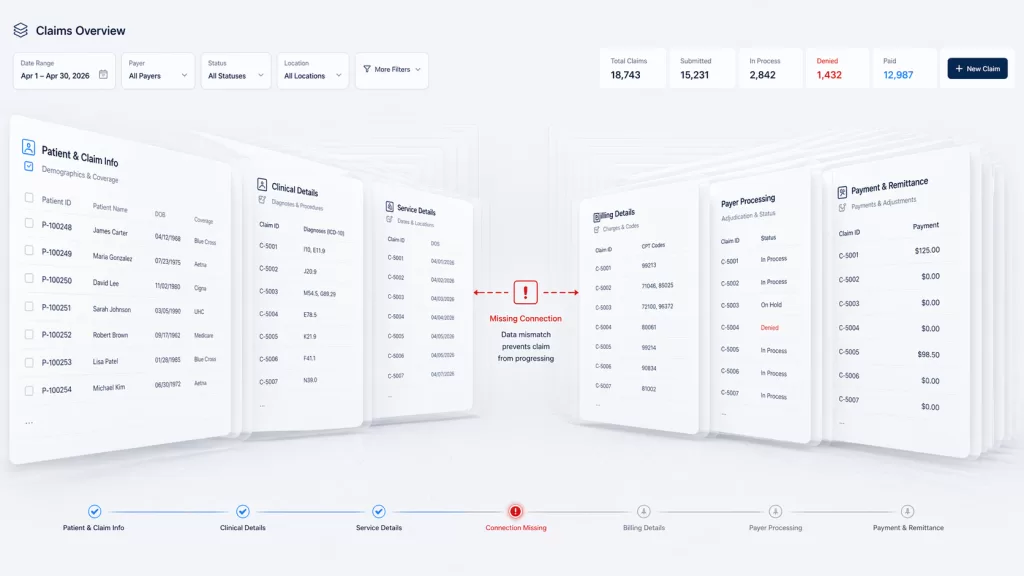
This lack of standardization creates three immediate problems:
- Reconciliation becomes more complex because payments no longer match original postings
- Staff must spend additional time researching the source of the adjustment
- Delays in response can lead to financial or compliance consequences
When a takeback is not clearly linked to a claim, it essentially sits unresolved in your system. That unresolved balance affects reporting, creates uncertainty in accounts receivable, and increases the likelihood of errors during posting and follow-up.
How Takebacks Are Typically Processed
Understanding how payers recover funds is critical because it determines your internal workflow.
| Takeback Method | What It Means Operationally |
|---|---|
| Automatic recoupment | Payer deducts the amount from future payments |
| Check request | Practice must issue a refund within a defined timeframe |
| Conditional recoupment | Payer requests a check but will auto-deduct if unpaid |
| ERA/EOB adjustment | Negative line item tied to a claim or payment ID |
Each of these requires a different response. The mistake many practices make is treating all takebacks the same, when in reality, the timing and process vary depending on the payer.
If your team does not clearly understand which method is being used, you risk either duplicating a refund or missing a required payment entirely.
The Financial and Compliance Risk Most Practices Miss
Takebacks are not just about giving money back—they carry real risk if mishandled.
If a payer requests a refund and it is not processed within the required timeframe, the balance can escalate. In some cases, it may be treated as an outstanding liability and sent to collections. That can affect your business credit and damage your relationship with the payer.
There is also reputational risk. Payers track provider behavior, and repeated delays or failures to respond to takebacks can impact how your practice is viewed operationally.

At the same time, automatically accepting every takeback without review creates a different problem—unnecessary revenue loss.
Why Investigation Is Non-Negotiable
Not every takeback is correct.
Some are straightforward, such as duplicate payments or coordination of benefits issues. In those cases, the reversal is expected and appropriate.
But others require deeper review. Missing documentation, incorrect payer assumptions, or processing errors can all lead to inappropriate takebacks.
This is where many practices fall into a reactive pattern—processing the adjustment without validating it.
A structured review process should always answer three questions:
- Was the original payment actually incorrect?
- Is there supporting documentation to defend the claim?
- Does the payer’s reason align with the clinical and billing data?
If the answer is unclear, further investigation is required. If the payer is incorrect, you have the right to dispute the takeback and provide supporting documentation.
Giving money back without verification is just as risky as ignoring the takeback entirely.
The Role of Timeliness in Managing Takebacks
Time is one of the most critical factors in managing retractions.
Payers typically provide a window to respond—whether that means issuing a refund or disputing the decision. If your team delays investigation, that window closes quickly.
This creates a difficult situation. You either rush a decision without proper review or miss the deadline entirely and lose the ability to respond effectively.
The practices that manage this well treat takebacks as priority work, not backlog work. As soon as a retraction is identified, it is assigned, investigated, and resolved within the payer’s timeframe.
This requires clear workflows and defined responsibilities.
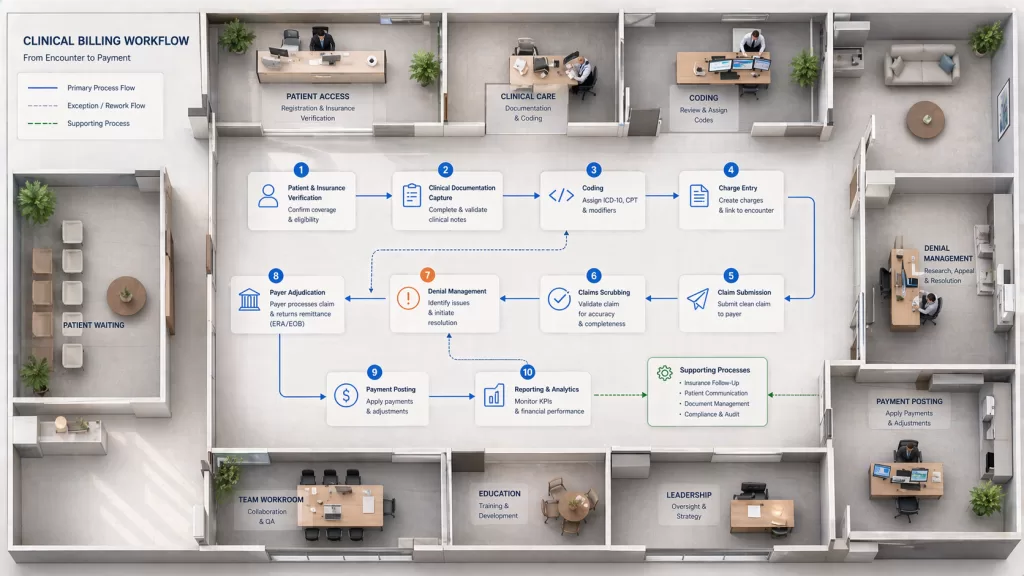
Where Internal Workflows Break Down
Most issues with takebacks are not caused by the payer—they are caused by gaps in internal processes.
Common breakdowns include:
- No defined ownership for reviewing and resolving takebacks
- Inconsistent monitoring of ERAs and incoming correspondence
- Lack of a tracking system for outstanding retractions
- Delays in communication between billing and finance teams
When these gaps exist, takebacks become reactive. They sit unresolved, get addressed inconsistently, or are handled too late.
Over time, this creates a cycle of financial inaccuracy and operational stress.
Building a Controlled Takeback Process
To manage takebacks effectively, your process needs structure and visibility.
That starts with tracking. Every takeback should be logged with the payer, amount, date received, method of recovery, and current status. Without tracking, it becomes impossible to manage volume or ensure timely resolution.
It also requires workflow clarity. Staff need to know exactly what to do when a takeback is identified—who investigates it, who decides whether to dispute or pay, and who completes the final step.
Finally, consistency matters. Each payer has different behaviors, and over time, patterns emerge. Documenting those patterns—how each payer handles takebacks—helps reduce confusion and speeds up decision-making.
Final Takeaway
Insurance takebacks are not rare events—they are a normal part of the revenue cycle. What determines their impact is how they are managed.
Without structure, they create confusion, delay reconciliation, and introduce financial and compliance risk. With a clear process, they become manageable and predictable.
The key is to treat takebacks as active revenue events, not passive adjustments. They require investigation, timely action, and consistent tracking.
When your team approaches them with that level of control, you protect both your revenue and your operational stability—even when payers reverse course.
