Medicare Telehealth Changes 2025: What Clinics Must Know
Medicare Telehealth Changes 2025
Effective October 1, 2025, the CMS telehealth guidelines 2025 roll back many COVID-era flexibilities. That means fewer covered services, tighter compliance rules, and a big shift for practices that rely on virtual care.
- Flexibilities end: Home-based telehealth visits won’t qualify for most specialties.
- Exceptions: Behavioral health, ESRD home dialysis, and acute stroke remain covered (with conditions).
- Originating site rules return: Patients must be in approved facilities or HPSA/rural areas.
- Provider limits: Only physicians, NPs, PAs, and some CNS can bill telehealth after the reset.
- Billing updates: POS 10 (home) retires; POS 02 (facility) remains active.
- Supervision changes: Virtual oversight for teaching physicians ends Dec 31, 2025.
- Audio-only scaled back: Limited to behavioral health, opioid treatment, and temporary codes.
This post breaks down what’s ending, what stays, and how to prepare so your clinic avoids denied claims and patient disruption.
The countdown is on, and this isn’t just another policy update buried in fine print. Medicare telehealth changes 2025 will take effect on October 1st, 2025, ending the COVID-era flexibilities that made virtual care so widely accessible. Clinics that don’t adjust now risk scheduling chaos and denied claims as the system snaps back to pre-pandemic rules.
These changes go far beyond minor billing adjustments. They reshape how patients connect, how providers bill, and which services can continue virtually. For many practices, it won’t be possible to deliver telehealth in the same way you have since 2020. You can read more about these updates directly from CMS here: Telehealth Policy Updates – HHS.gov
From Flexibility to Compliance: Why the Reset Matters
If you’ve been watching the clock tick toward September 30th, you know there’s no safety net this time—CMS isn’t signaling another extension. That means a short window to review workflows, retrain schedulers, and prepare for a pivot back to tighter compliance.
Think of this guide as your roadmap. We’ll break down what’s ending, what’s staying, and how to prepare without losing revenue or patient trust.
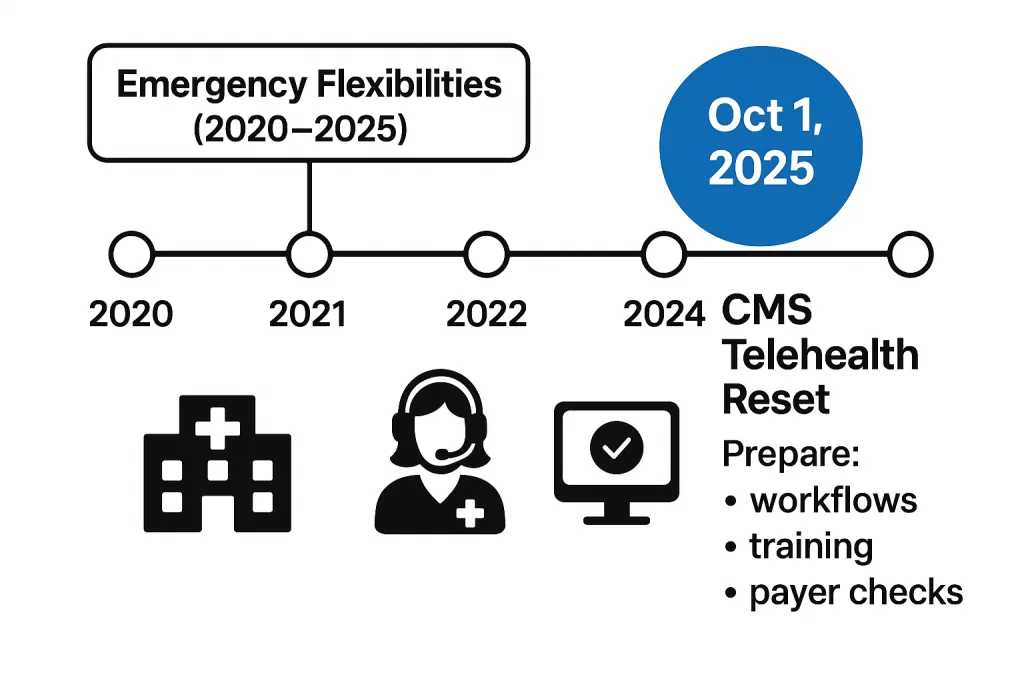
Table of Contents
Why Medicare Telehealth Flexibilities End in 2025
Back in 2020, CMS opened the telehealth floodgates. Hospitals were packed, waiting rooms were risky, and patients needed safe ways to connect. So Medicare bent the rules, added temporary codes, and paused the usual restrictions. Those changes became the backbone of virtual care. But the Medicare telehealth changes 2025 roll us back to pre-pandemic standards. The new CMS telehealth guidelines 2025 mark the end of that emergency flexibility and a return to tighter compliance.
Now it’s time for the reset. On October 1st, 2025, CMS is pulling back to something closer to the pre-pandemic telehealth rules. The agency made it clear from day one that these changes were temporary. Providers may have gotten comfortable billing telehealth from anywhere, but the official guidance never promised a forever pass.
No More Extensions: CMS Telehealth Guidelines 2025 Take Effect
The shift isn’t meant to punish clinics. Instead, CMS argues it’s about compliance, oversight, and making sure virtual care is delivered in the right settings. That means some specialties will still thrive under the new system, while others will hit roadblocks. The Medicare telehealth changes 2025 aren’t a total shutdown. They’re more of a rollback, with carve-outs for conditions like end-stage renal disease, acute stroke treatment, and behavioral health services.
If you run a practice that leans heavily on telehealth, the most important takeaway is this: the CMS telehealth guidelines 2025 are finalized, and unless Congress steps in with an eleventh-hour extension, October 1st marks the official cutoff.
Which Specialties Keep Telehealth Under CMS Telehealth Guidelines 2025
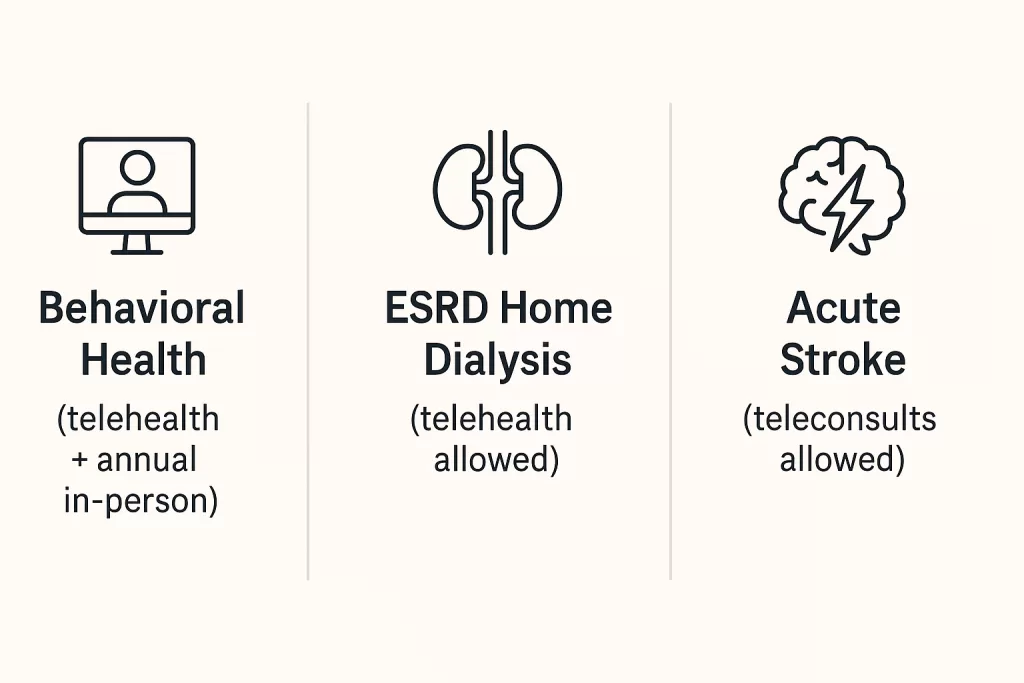
Not every service is disappearing when the Medicare telehealth changes of 2025 take hold. A few key exceptions will keep their virtual pathways open, though the rules will look different than the wide-open pandemic era.
The CMS telehealth guidelines 2025 carve out some exceptions. Behavioral health services, including mental health and substance use disorder treatment, remain covered through telehealth. The catch? Patients must have an in-person visit within six months of their first telehealth session, and at least once a year after that. Under the Medicare telehealth changes 2025, only three categories stay fully supported: behavioral health, ESRD dialysis, and acute stroke treatment.
Critical Access Matters: Carve-Outs in Medicare Telehealth Changes 2025
Another exception is end-stage renal disease (ESRD). Patients receiving home dialysis can still be supported virtually. This carve-out reflects how critical access is for people managing chronic conditions that don’t always require face-to-face visits.
Acute stroke treatment is also being conducted through telehealth. The need for rapid evaluation and decision-making makes virtual access essential here. It’s one of those rare cases where technology truly changes outcomes, and CMS is keeping it intact.
To make it easier to compare what’s sticking versus what’s expiring, here’s a quick reference:
| Specialty / Condition | Telehealth Allowed After Oct 1, 2025 | Extra Requirements |
|---|---|---|
| Behavioral / Mental Health | Yes | In-person visit within 6 months, then annually |
| ESRD / Home Dialysis | Yes | No major changes |
| Acute Stroke Treatment | Yes | No major changes |
| Other Specialties | Mostly No | Must meet rural + site limits |
These exceptions may sound generous, but they’re narrow. If your practice doesn’t fall into one of these buckets, you’ll be back under the stricter CMS telehealth guidelines in 2025. That means more planning, more scheduling changes, and more patient education to keep everything on track.
Telehealth Originating Site Rules Return in 2025
One of the most jarring parts of the Medicare telehealth changes 2025 is the return of originating site restrictions. During the pandemic, patients could hop on a video call from their couch and still have it covered. Starting October 1st, that option disappears for most specialties.
The new CMS telehealth guidelines 2025 make originating site rules matter again. Patients must be physically present in an approved location—such as a hospital, skilled nursing facility, or rural health clinic—to qualify for coverage. For most specialties, the home will no longer be valid. Only a few exceptions survive under the Medicare telehealth changes 2025, including behavioral health services and ESRD dialysis visits.
This is where convenience takes a big hit. For urban and suburban patients, the rule may feel like a total shutdown. Most don’t qualify for a rural or Health Professional Shortage Area (HPSA), and without those designations, telehealth coverage won’t apply. For practices, this means patient education has to happen now. You can’t wait until denied claims start stacking up.

Here’s a snapshot to clarify how the originating site rules shake out:
| Patient Location | Covered After Oct 1, 2025? | Notes |
|---|---|---|
| Home | No | Except for behavioral health, ESRD dialysis, acute stroke |
| Rural/HPSA Clinic | Yes | Must be in approved shortage area |
| Hospital | Yes | Approved originating site |
| Skilled Nursing | Yes | Approved originating site |
The message is clear: geography matters again. If your patients live in a city and expect to continue virtual visits from home, they’re in for a surprise. For practices, this involves reworking scheduling, updating scripts for front office staff, and making sure patients don’t get blindsided.
Which Providers Can Bill Telehealth Under CMS Telehealth Guidelines 2025
The Medicare telehealth changes 2025 don’t just limit where patients can be. They also narrow down who can bill for telehealth. Before the pandemic, the list was short. Then the flexibilities opened the door to more provider types. Now, CMS is slamming that door halfway shut again.
The Medicare telehealth changes 2025 don’t just limit patient settings—they also tighten who can bill telehealth. Starting October 1st, only physicians, nurse practitioners, physician assistants, and some clinical nurse specialists qualify. The CMS telehealth guidelines 2025 cut out PT, OT, and SLP providers entirely unless Congress extends coverage. This narrowing means practices need to audit schedules now to prevent denied claims.
Here’s how it looks when broken down:
| Provider Type | Eligible After Oct 1, 2025? | Notes |
|---|---|---|
| Physicians | Yes | Must follow site + geography rules |
| Nurse Practitioners (NPs) | Yes | Same restrictions apply |
| Physician Assistants (PAs) | Yes | Same restrictions apply |
| Clinical Nurse Specialists | Yes | Limited scope |
| PT, OT, SLP | No | Lose telehealth reimbursement unless Congress acts |
| Other Allied Health Providers | No | Coverage ends unless extended |
For physical therapy, occupational therapy, and speech-language pathology, the news is rough. Unless lawmakers step in, these professionals lose Medicare telehealth reimbursement entirely. It’s one of the most painful parts of the rollback, especially since many of these providers proved how effective remote sessions could be.
This is where compliance meets cash flow. If your practice schedules the wrong provider for a telehealth visit, the claim will almost certainly get denied. That means it’s time to audit your workflows, train your schedulers, and verify which staff can continue to provide virtual care.

CMS Telehealth Changes 2025 for Teaching Physicians
One under-the-radar change in the Medicare telehealth changes 2025 affects teaching physicians. During the pandemic, virtual supervision counted. A physician could oversee residents remotely, and CMS reimbursed it. But the new CMS telehealth guidelines 2025 end that flexibility on October 1st, requiring in-person presence for most supervision. Programs relying on remote oversight need to plan now, because by December 31st, 2025, even the temporary grace period runs out.
Under the new CMS telehealth guidelines 2025, teaching physicians must once again be physically present for most resident supervision. Virtual oversight won’t count outside of very limited situations. That means programs relying on remote supervision will have to change schedules and expectations quickly.
</div></figure>
<!– /wp:embed –>
Residency Programs Face Big Changes in Telehealth Oversight
There is one reprieve. CMS is allowing teaching physicians flexibilities to stay in place until December 31st, 2025. This gives residency programs a few extra months to adapt before the rule shuts completely. After that, the pre-pandemic standard comes back into full force.
Why does this matter? Because residency programs aren’t just training grounds—they’re part of daily patient care. If supervision rules shift, it affects coverage, staffing, and even patient wait times. Practices connected to teaching hospitals need to prepare now, not later. Waiting until January could mean disrupted workflows and denied billing.
The bottom line is clear: virtual supervision doesn’t survive past 2025. If your practice or program leaned on it, plan your transition now so you’re not scrambling when the window closes.
Audio-Only Telehealth Services Under Medicare 2025
Phone calls won’t cut it anymore. The Medicare telehealth changes 2025 scale back audio-only services to very limited scenarios. The CMS telehealth guidelines 2025 allow them only for behavioral health, opioid treatment programs, and select codes like caregiver training. For most specialties, audio-only reimbursement disappears, forcing a return to video or in-person visits.
CMS is keeping audio-only for behavioral health visits, opioid treatment programs, and a handful of specialized services. If you’ve been using phone visits across multiple specialties, those days are over. Most practices will need to shift patients back to video or in-person visits to stay compliant.
Temporary service codes also remain in play—at least for a while. Caregiver training, some preventive counseling codes, and a few patient education services are still billable through 2025. These codes are expected to be reviewed again when the 2026 Medicare final rule comes out later this year. Translation: they could vanish if CMS decides not to make them permanent.
Here’s a quick snapshot:
| Service Type | Status in 2025 | Notes |
|---|---|---|
| Behavioral Health (Audio-Only) | Allowed | In-person requirement still applies annually |
| Opioid Treatment Programs | Allowed | Phone visits covered |
| Caregiver Training Codes | Temporary | Approved through 2025 |
| Preventive Counseling | Temporary | Review pending for 2026 |
| General Audio-Only Services | Not Allowed | Must use video or in-person |
The tricky part is communication. Patients who are used to quick phone visits may not realize the rules are changing. If your team doesn’t explain the limits ahead of time, expect frustration when the bill comes back denied.
The safe move? Audit your telehealth appointment types, flag audio-only codes that are disappearing, and retrain staff on when phone visits are still compliant. Otherwise, your claims could be in trouble before the year ends.
Medicare Telehealth Billing Codes: POS 10 Retires in 2025
Billing teams, this is where the Medicare telehealth changes 2025 get tricky. The new CMS telehealth guidelines 2025 bring a major coding shift that could derail claims if you’re not ready. Until now, the Place of service code has been the go-to for telehealth visits conducted at a patient’s home. But after September 30th, 2025, that code expires, leaving only POS 02 for approved facilities and rural settings.
From now on, the main option left is POS 02—but only when the patient is in an approved originating site like a clinic, hospital, or skilled nursing facility. For most patients, the home won’t qualify anymore, so you’ll need to check both geography and setting before coding.
Here’s how it looks at a glance:
| Place of Service Code | Status After Oct 1, 2025 | When to Use It |
|---|---|---|
| POS 10 (Patient Home) | Ends Sept 30, 2025 | No longer billable |
| POS 02 (Telehealth Facility) | Remains active | Use when patient is in an approved originating site |

This may sound like a small change, but it’s a revenue landmine. If schedulers don’t adjust appointments or coders forget to swap POS codes, Medicare will deny the claim. And once denials pile up, fixing them is a painful, time-consuming process.
The safest path is to start training staff now. Create new cheat sheets for coders, update your EHR workflows, and have billing teams test claims if possible. The sooner everyone knows that POS 10 retires and POS 02 remains, the smoother the transition will be.
How Practices Should Prepare for CMS Telehealth Guidelines 2025
The worst mistake is waiting. The Medicare telehealth changes 2025 take effect October 1st, and under the new CMS telehealth guidelines 2025, unprepared practices will see chaos and denied claims. Preparation starts now: review scheduled patients, train staff, and notify patients about what qualifies. Waiting until after denials hit is too late.
First, run a report of every patient currently booked for telehealth visits after September 30th. Flag those encounters and check whether they’ll still qualify under the CMS telehealth guidelines 2025. If the answer is no, start rescheduling in-person visits before patients arrive online for unpaid appointments.
Second, patient communication is critical. Many patients assume telehealth is here forever. They’ll need clear explanations about why Medicare is changing the rules and what it means for them. A quick call, a portal message, or even a mailed notice can prevent surprises. The goal is to prevent frustrated patients from finding out the hard way that their home telehealth visit won’t be covered.
Third, train your staff. Front desk schedulers, billers, and providers all need to be on the same page. If a patient calls asking for a telehealth appointment, your staff should know immediately whether that request fits under the new guidelines. That saves time, reduces errors, and keeps trust intact.
Finally, remember that commercial insurers don’t all follow Medicare’s lead on the same timeline. Some will align on October 1st, while others may wait until January 1st, 2026. That means you’ll need to do payer-specific due diligence. Checking those policies now ensures you won’t get blindsided when the new year rolls around.
Frequently Asked Questions About Medicare Telehealth Changes 2025
What are the Medicare telehealth changes in 2025?
Starting October 1, 2025, CMS telehealth guidelines roll back most COVID-era flexibilities. Home-based visits will no longer qualify for most specialties, and originating site restrictions return. Only certain conditions, like behavioral health, ESRD dialysis, and acute stroke treatment, remain fully supported under Medicare telehealth coverage.
Which providers can bill for telehealth under the 2025 rules?
Medicare telehealth billing in 2025 is limited to physicians, nurse practitioners, physician assistants, and some clinical nurse specialists. Physical therapy, occupational therapy, and speech-language pathology are excluded unless Congress passes an extension. Practices need to audit schedules to avoid denied claims once the new guidelines take effect.
What specialties keep telehealth coverage in 2025?
Three categories remain covered under Medicare telehealth changes: behavioral health services, ESRD dialysis, and acute stroke treatment. Behavioral health requires at least one in-person visit annually. These carve-outs reflect CMS’s focus on critical and high-impact care while removing broader access created during the pandemic emergency period.
What happens to audio-only telehealth in 2025?
Audio-only services are significantly reduced. Starting October 1, 2025, Medicare covers phone visits only for behavioral health, opioid treatment programs, and a few temporary caregiver training or counseling codes. Most other specialties must switch back to video or in-person visits to meet CMS telehealth billing compliance requirements.
How do originating site rules affect patients in 2025?
Under CMS telehealth guidelines 2025, patients must be in approved facilities such as hospitals, rural clinics, or skilled nursing centers for coverage to apply. Home visits will not qualify, except for behavioral health, ESRD dialysis, and acute stroke. Geography matters again, particularly for urban patients.
What happens to POS 10 and POS 02 billing codes?
Medicare is retiring POS 10 (telehealth in patient homes) after September 30, 2025. POS 02 remains for approved facilities and rural sites. Practices must update scheduling and coding workflows to prevent denials. Training staff now ensures smoother billing transitions when the new CMS telehealth rules take effect.
How do the new rules impact teaching physicians?
Teaching physicians lose the flexibility to supervise residents virtually. Starting October 1, 2025, in-person oversight is required, with a grace period until December 31, 2025. After that, remote supervision no longer qualifies for Medicare reimbursement, requiring residency programs to adjust coverage, schedules, and compliance procedures.
Will commercial insurers follow Medicare’s telehealth changes?
Not immediately. While some insurers may align with Medicare on October 1, 2025, others will wait until January 1, 2026. Practices should review payer-specific telehealth policies and timelines now. Preparing ahead avoids disruptions and ensures billing compliance across both Medicare and commercial insurance carriers.
Telehealth Beyond 2025: What to Expect in Medicare’s 2026 Final Rule
The Medicare telehealth changes 2025 may feel like a step backward, but they’re just the start. CMS has already signaled that the 2026 Medicare final rule will revisit service codes, supervision flexibilities, and reimbursement policies. While the CMS telehealth guidelines 2025 tighten restrictions, the coming updates may expand access again—especially if Congress acts on PT, OT, and SLP telehealth bills.
For now, we know a few things. Temporary service codes—like caregiver training and certain counseling visits—are on the table for review. CMS may decide to make some permanent, while others could quietly disappear. Providers who rely on these codes should keep a close eye on the announcements expected in Q4 of 2025.
Will Congress Expand Telehealth Beyond CMS Guidelines 2025?
There’s also growing momentum to expand telehealth in targeted areas. Lawmakers have floated bills to restore access for PT, OT, and SLP providers, but nothing is guaranteed. If you serve patients in those fields, advocacy and professional organizations will be your best resource to stay informed.
The big unknown is whether geography and originating site restrictions will loosen again. Right now, CMS shows no signs of backing off. The home remains excluded for most specialties, and urban patients are the ones most affected. Unless Congress steps in, those rules will likely stand for the foreseeable future.
How Practices Can Thrive in a Regulated Telehealth Era
So, what should practices do? Stay alert. Monitor CMS announcements, subscribe to payer updates, and set internal reminders to review new rules every quarter. Telehealth isn’t vanishing, but it’s entering a new, more regulated era. The practices that adapt quickly—by training staff, educating patients, and building flexible workflows—will be the ones that thrive.
The pandemic may have given us a wide-open telehealth playground, but CMS telehealth guidelines 2025 and beyond are more like an obstacle course. Learn the rules, play smart, and you’ll still find ways to deliver care without missing a beat.
