Surviving the Impacts of the Federal Government Shutdown on Healthcare
What happens when Washington stops working—but your patients don’t? The impacts of the Federal Government Shutdown on Healthcare stretch far beyond D.C. offices. They reach your billing department, your Medicare payments, and your cash flow. Claims are slow, some systems queue, and routine workflows hit bottlenecks; even the most routine processes get tangled in red tape.
Key Takeaways
- CMS continues limited operations during shutdowns, but Medicare claims are delayed.
- Claim submissions should continue during shutdowns to stay early in the queue.
- Shutdowns impact provider enrollment, appeals, audits, and vendor communication.
- Financial forecasting and reserve planning are key to surviving cash flow gaps.
- Clean claims and automated systems reduce backlogs and payment errors.
- Effective communication with staff, patients, and MACs helps build trust during times of uncertainty.
- Recovery after reopening requires detailed reconciliation and proactive follow-up.
If you’ve ever wondered how to keep your practice steady during a freeze, this guide breaks down what to expect from Medicare payment delays in 2025 and how to protect your financial stability when government operations go dark.
Table of Contents
What the Federal Shutdown Means for Healthcare and Medicare
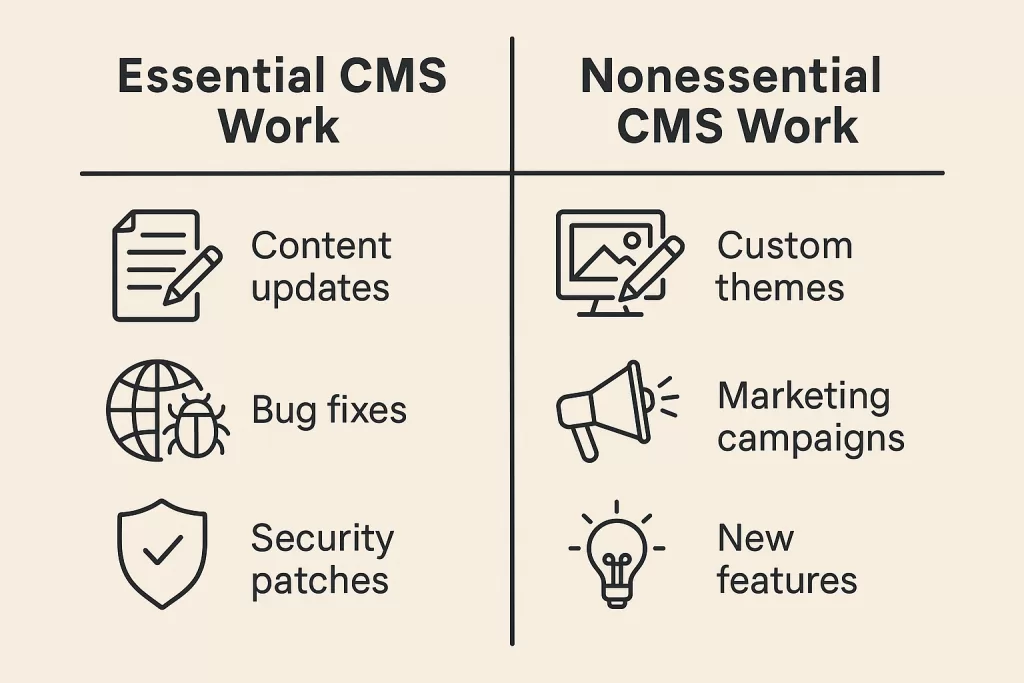
When a shutdown hits, agencies pause or reduce non-excepted work; only “excepted” (and other-funded) activities continue. Even critical programs like Medicare feel the drag because systems depend on staffing, oversight, and appropriations. During a lapse, fewer people are available to supervise operations, which can create backlogs and delays in adjudication and support functions (OPM guidance; HHS FY2026 Contingency Staffing Plan).
Claims still reach Medicare Administrative Contractors (MACs), but those contractors rely on CMS systems and human oversight. When furloughs reduce staffing, manual reviews slow and bottlenecks pile up—producing a practical processing delay that hits provider revenue first (HHS contingency plan).
| Essential/Excepted Work | Non-excepted or Paused Work |
|---|---|
| Claim payments and basic adjudication | Many appeals/redeterminations |
| Emergency public health responses | Some provider enrollment updates |
| Ongoing funded audits in progress | New pilots/rulemaking not otherwise funded |
| Core system maintenance | Portions of prior authorization and program support |
Context note: HHS’s plan indicates a substantial share of staff may be furloughed during a lapse, which can slow even excepted work due to limited human oversight (HHS contingency plan).
Open Enrollment During a Shutdown
Medicare Open Enrollment runs Oct 15–Dec 7; plan changes generally take effect Jan 1 (Medicare.gov).
| Status | What Happens During Shutdown | What to Expect After Reopening |
|---|---|---|
| Initial claim processing | Active, but slower | Gradual normalization |
| Appeals / Redeterminations | Often delayed or queued | Multi-week backlog |
| Provider enrollment changes (PECOS) | Often delayed/queued | Slow verification |
| Audit responses | Limited | Significant delay |
Managing the Ripple Effect of Medicare Payment Delays
If you’ve ever watched a row of dominoes fall, you already know what’s coming next. The impacts of the federal government shutdown don’t stop at Washington — it rolls right into your clinic’s finances. When Medicare payment delays start stacking up, payroll tightens, vendor payments stall, and patient scheduling becomes a juggling act.
This kind of government shutdown disruption affects both small and large practices. The key is staying calm, informed, and strategic. Here’s how to stay ahead and protect your operations during CMS slowdowns.
Adjusting Financial Forecasts During a Shutdown
Now’s not the time to coast on autopilot. The shutdown directly affects cash flow, and a Medicare claim processing slowdown can leave practices short for weeks — even after CMS reopens. Remember, once furloughed staff return, it can take months to clear the backlog.
So what should you do? Start with a realistic cash flow forecast. Pull your financial reports and plan for at least a 30% delay in expected Medicare payments. That buffer helps you prepare before problems surface.
Whether you use advanced software or a spreadsheet, track each payment’s usual timing and extend those dates. This kind of healthcare financial planning during the shutdown gives you control when everything else feels unpredictable.
And if you’ve been eyeing new equipment or EHR upgrades, hold off. Conserve cash until CMS operations fully normalize and payments stabilize.
Why You Should Still Submit Claims Immediately
A common question during shutdowns is whether you should hold claims until CMS reopens. The short answer? Absolutely not.
The shutdown doesn’t stop claim acceptance — it just slows processing. Medicare administrative contractors still receive files, and they’re processed in the order received. If you wait, your claims land at the bottom of a massive post-shutdown queue.
Submitting now, with “clean” claims, gives you the best chance to keep revenue trickling in. Even if payments are delayed, being early helps you recover faster once Medicare administrative contractor delays clear.
Don’t stall. Keep operations moving, clean claims submitted, and your place secured in the processing line.
Preparing for Extended Delays
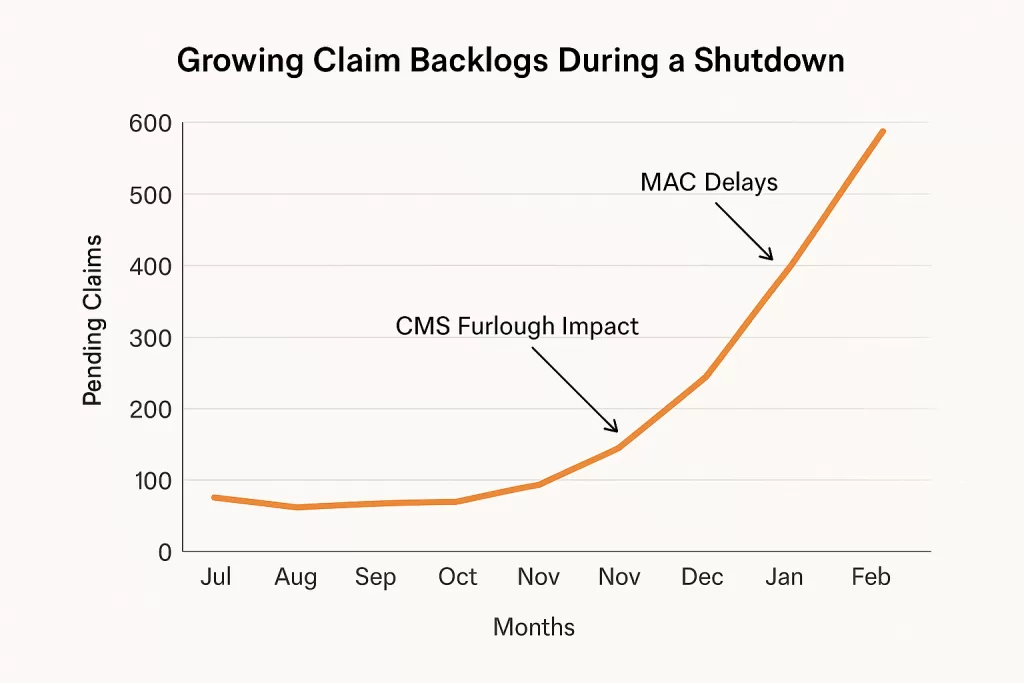
What happens if the shutdown stretches into weeks—or even months? The impacts of the Federal Government Shutdown on Healthcare start compounding over time.
The longer CMS staff are furloughed, the more severe Medicare payment delays become, and many commercial insurers adjust timelines alongside CMS; verify specifics per contract. When federal reimbursements slow, private payers follow, creating a systemwide impact that can strain every part of your operation.
Prepare by keeping a dedicated reserve account for payroll or critical expenses. Communicate openly with your staff if cash flow tightens temporarily—transparency builds trust and keeps morale high.
And remember, your billing team will feel this pressure too. Offer support, not blame, as they manage Medicare administrative backlogs and patient inquiries. Leadership during a slowdown determines the strength of your practice when CMS returns to full capacity.
What to Expect When the Government Reopens
When the shutdown finally ends, the impacts don’t disappear overnight; they linger. CMS and HHS will triage thousands of pending cases, prioritizing emergency payments and compliance tasks first. That means Medicare claim adjudication delays can persist for weeks after government operations resume.
Practices that continued submitting claims during the shutdown will recover fastest because their claims are already in queue. Those that waited will find themselves at the back of a very long line once Medicare administrative contractor delays begin clearing.
Expect at least a month of unstable reimbursement cycles before things normalize. CMS will issue updates outlining when Medicare appeals and redeterminations on hold will resume and when provider enrollment delays PECOS will start clearing. CMS notes funded activities continue; non-funded actions may queue until appropriations resume. Staying informed helps you forecast cash flow and plan staffing more confidently during this recovery window.
How to Recover Once CMS Reopens

When CMS finally returns to full operations, the impacts of the federal shutdown enter their most critical phase—recovery. It’s tempting to exhale and move on, but this is where the real work begins. Piles of backlogged claims, mismatched payments, and delayed reassignments can cause lingering Medicare cash flow disruption for weeks.
Use the reset period to go heads-down on fundamentals: verify payments, reconcile every remittance, and confirm your systems are syncing correctly with clearinghouses and contractors. Backlogs won’t disappear overnight, and some CMS functions may take time to return to full speed—so tightening your internal controls now prevents weeks of downstream errors.
The good news? With a focused plan and proactive communication, your practice can turn recovery chaos into long-term operational strength. The next few steps will show you how to do exactly that.
Tracking and Reconciling Claims After Reopening
When payments finally start rolling in, please don’t assume they’re all correct. Due to the chaos, some claims may be paid partially, duplicated, or even skipped.
Start by running a claims aging report. Separate pending payments from posted ones. Then, cross-reference your ERA (Electronic Remittance Advice) files against your original submissions. If you find mismatched payments, log them for follow-up.
Here’s a simple table layout that helps keep your tracking clean and easy:
| Claim Type | Submitted Date | Expected Payment | Actual Payment | Follow-Up Needed |
|---|---|---|---|---|
| Standard Medicare | Sept 12 | $480.00 | $480.00 | No |
| Corrected claim | Sept 25 | $1,230.00 | $0.00 | Yes |
| Appeal pending | Aug 30 | $860.00 | $0.00 | Yes |
Using this system helps you spot what still needs attention as CMS furlough impact resolves. If you’re short-staffed, this is where temporary billing help or a consultant can be worth every penny.
Managing Cash Flow After Reopening
When the first payments finally arrive, they might look like a windfall—but don’t be fooled. Those deposits are the result of backlogged claims catching up, not new growth. The healthcare impact of the federal shutdown can still cause irregular cycles and Medicare cash flow disruption even weeks after reopening.
Keep your spending conservative. Redirect a portion of incoming funds into a reserve account to build stability for the next potential government shutdown event. If this experience revealed anything, it’s that resilience comes from preparation.
A smart rule of thumb: set aside 10–15% of your average Medicare income for emergencies. That reserve will help you weather the next round of delays without cutting payroll or patient services.
Communicating with MACs and Vendors After Reopening
Once CMS resumes full operations, Medicare administrative contractor delays will take time to resolve, but communication channels will reopen quickly. Contact your MAC through their provider portal or help desk and confirm that your pending claims, Medicare appeals and redeterminations on hold, and enrollments are properly queued.
Touch base with your clearinghouse and billing vendors too. Many release post-shutdown updates that explain how to re-sync ERA files, correct submission errors, and handle system backlogs caused by CMS furlough impact.
Reconnecting early helps prevent duplicate work and missed claims. It’s also a smart moment to check in with payer representatives, as proactive communication can move your practice ahead of slower competitors still catching up.
Reviewing Denials and Redeterminations
Once CMS operations resume, expect a surge of old claim responses, appeals, and redeterminations coming through at once. The impacts of the Federal Government Shutdown on Healthcare become painfully clear here—denials pile up, and some no longer match your updated records.
Others may be auto-denied due to mismatched data or expired timeframes, making accurate documentation critical. Keep your Medicare appeals and redeterminations on hold spreadsheet current and organized.
If you receive a denial caused by claim adjudication delays, log all timestamps — submission, acknowledgment, and notice date. CMS often issues reconsideration windows for shutdown-related cases.
Bottom line: document every detail. Strong records protect your revenue once Medicare audit delays and system errors start surfacing after the shutdown.
Updating PECOS Records After a Shutdown
One of the most overlooked areas is the provider credentialing stall shutdown. Provider enrollment delays in PECOS can extend well beyond the reopening week as CMS verifies every pending record.
Check your PECOS dashboard weekly. If your application shows “pending,” it’s likely still working through Medicare administrative backlogs. However, if there’s no update after 30 days, follow up directly with your MAC’s provider-enrollment department.
Also, confirm your NPI and reassignment data match your current records. During a CMS furlough impact, data validation halts, and mismatched entries can trigger rejections or missing reassignment links. Fixing these now prevents more processing delays later.
Planning for the Next Federal Shutdown
It might sound pessimistic, but the truth is this won’t be the last time a Federal Government Shutdown affects your clinic. Building a shutdown resilience plan now ensures smoother operations next time.
Focus on these essentials:
- Financial buffer: Keep at least one to three months of reserves to handle Medicare payment delays or similar disruptions.
- Automation: Use automated scrubbing and claim submissions so billing doesn’t freeze if CMS operations slow again.
- Dashboards: Track real-time claim aging and Medicare cash flow disruption in your EMR or accounting tools.
- Training: Equip staff with step-by-step workflows for slowdowns, appeals, and reprocessing.
Preparation prevents panic. Each plan you build today helps reduce the chaos that inevitably follows another government shutdown disruption in healthcare.
Supporting Staff and Patients After a Shutdown
The impacts of the Federal Government Shutdown don’t stop at paperwork—it affects people. After months of stress and uncertainty, your staff needs recovery time too. Use the post-shutdown lull to recognize their effort and rebuild morale. Even small gestures—a team lunch, a thank-you note, or a brief afternoon off—show leadership that values human resilience.
Patients also feel the strain. Some may face delayed authorizations or unclear balances. Communicate openly through your website, portal, or appointment reminders. A short update explaining that CMS operations being shut down caused national slowdowns demonstrates professionalism and empathy.
Celebrating the Comeback
When payments stabilize and operations normalize, celebrate your comeback. The impacts of the Federal Government Shutdown tested every clinic’s patience, planning, and adaptability. You kept claims moving, employees paid, and patients supported—and that deserves recognition.
Now channel that experience into long-term growth. Review your workflows, note which systems held up best during the Federal Government Shutdown, and strengthen them for the future. Next time Washington pauses, your practice will already have the resilience—and the playbook—to keep going strong.
Key Lessons From the Federal Shutdown in Healthcare

After weeks of tension, delayed payments, and endless refreshes of the CMS portal, one thing is crystal clear — the government shutdown’s impacts extend far deeper than most expect. What started as a budgeting standoff in Washington quickly turned into a slowdown that touched every clinic, billing department, and patient waiting for their claims to clear.
Although the Medicare claim processing slowdown has been painful, it has also taught valuable lessons about resilience. Let’s wrap this up with what every healthcare organization — from solo practitioners to large groups — can carry forward.
Medicare Isn’t Invincible
It’s easy to think of Medicare as an unstoppable machine that always keeps running. But the recent shutdown revealed that even “essential” systems rely on people. When employees are furloughed, the human element disappears, and the gears of Medicare turn much more slowly.
That’s why the payment delays hit so hard. The system continued to run, albeit inefficiently. Claims still moved — just at a crawl. For every provider who assumed their payments were “guaranteed,” this was a wake-up call to build backup plans.
Proactive Providers Survive Best
The clinics that fared best during the CMS furlough impact were those that planned early. They forecasted lower revenue, submitted claims without delay, and maintained open communication with patients and payers. They treated the shutdown like a storm they could see coming.
Those who waited — or tried to “ride it out” — ultimately faced the brunt of the Medicare administrative contractor delays. It’s a pattern: the more proactive you are, the less painful the catch-up period becomes.
Clean Claims Save the Day
Every provider who got paid the fastest during this crisis had one thing in common: clean, error-free claims. That might sound obvious, but under the Medicare claim processing slowdown, it’s gold.
A small typo or mismatched code could add weeks to an already delayed payment. Clean claims glide through the system because they don’t need manual review — and with fewer CMS workers, that’s your best bet for quick payment.
Telehealth Needs a Safety Net
The telehealth reimbursement uncertainty that surfaced during this shutdown revealed a bigger problem — reliance on temporary policies. With CMS rulemaking on pause, many providers found themselves unsure whether certain virtual visits would be reimbursed at all.
The takeaway? Never base your business model on a government flexibility that could vanish overnight. Continue offering telehealth for patient care, but balance your service mix to maintain stability.
Communication Is Currency
Whether it’s your staff, your patients, or your payers, consistent communication can make or break trust during a crisis.
When Medicare payment delays started, some practices stayed silent — and that only fueled confusion. Others took the opposite approach: they informed patients that delays were systemic, updated their websites, and reassured staff about payroll timing.
Clear communication doesn’t fix the problem, but it softens the blow. It shows leadership, transparency, and empathy — traits that outlast the crisis.
Forecasting Is a Survival Skill
In healthcare, most owners think of forecasting as something finance teams do once a year. But in times like these, it’s a survival skill.
Your ability to anticipate the impacts of a federal shutdown separates the clinics that panic from those that pivot. Use simple models — even spreadsheets — to project how your cash flow changes when payments lag.
Private Payers Follow the Leader
This one caught a few people by surprise: Medicare claim processing delays don’t stay inside Medicare’s walls. Private payers often mirror CMS policy changes, and during the shutdown, that connection became obvious.
Many insurers delayed adjustments to their reimbursement rates because CMS hadn’t finalized new rules. Some even paused complex claims “pending clarification.” When Medicare sneezes, private insurance catches a cold.
Always Have a Plan B
If this shutdown shows anything, it’s that you can’t control the system — only your response to it.
Every practice should have a written contingency plan: how to operate when federal systems slow down, who handles patient care, and how billing continues if portals freeze. Preparation turns panic into a checklist.
Frequently Asked Questions About the Impacts of the Federal Government Shutdown on Healthcare
How does a federal shutdown affect healthcare operations?
A federal shutdown disrupts normal agency workflows, especially within CMS and HHS. While essential services like Medicare claims continue, staffing furloughs slow processing, delay payments, and pause appeals or enrollments. Clinics often experience reduced cash flow and administrative backlogs that take weeks to clear even after the government reopens.
Will Medicare still pay providers during a shutdown?
Yes, but slower than usual. Medicare administrative contractors continue limited operations, so claims can still process—but at a crawl. Human oversight, prior authorizations, and audits often pause. Providers should expect delayed reimbursements and maintain reserves or flexible payment schedules to avoid payroll and vendor issues during the disruption.
Should clinics continue submitting claims during the shutdown?
Absolutely. Claims are processed in the order they’re received, even if delayed. Submitting “clean” claims promptly ensures your place in line when processing resumes. Waiting to file can push your payments further back once CMS reopens and begins clearing its backlog, making delays even longer.
How can healthcare providers prepare for extended shutdown delays?
Providers should build financial buffers, delay major expenses, and communicate transparently with staff and patients. Track claim aging reports, forecast cash flow, and set aside emergency reserves for payroll or rent. Preparation—rather than reaction—keeps a practice stable even when federal reimbursements stall.
What happens to provider enrollment applications during a shutdown?
Provider enrollment activities through PECOS often pause during a shutdown. Applications remain pending until CMS staff return. Once operations resume, CMS clears backlogs in order of receipt, so monitoring your PECOS dashboard and following up after 30 days is key to preventing further credentialing delays.
How should clinics manage operations once CMS reopens?
Once CMS reopens, verify claim accuracy, reconcile remittances, and check for underpayments or denials. Communicate with your MACs and vendors to confirm everything is queued correctly. Prioritize clean claim submissions and appeal reviews. Financial recovery takes time, but staying proactive helps restore normal revenue flow faster.
What lessons can practices learn from past shutdowns?
Shutdowns reveal weak points in cash flow, communication, and claim accuracy. Practices that forecast revenue, automate claim tracking, and maintain reserves fare best. Every shutdown reinforces one truth: preparation and proactive planning are the most effective shields against systemic slowdowns in healthcare reimbursement.
How can clinics prevent future disruptions from hurting finances?
Build resilience by keeping at least one month’s expenses in reserve, automating billing processes, and training staff on contingency plans. Establish clear communication with payers and patients early. With these systems in place, the next healthcare impact of a federal shutdown won’t catch your clinic off guard.
How can clinics prepare for the Impacts of the Federal Government Shutdown on Healthcare?
Build a cash-reserve target (10–15% of average Medicare receipts), keep clean-claim workflows running, and pre-write contingency steps for appeals, enrollment follow-ups, and ERA reconciliation. During a lapse, claims can still be received and processed in order, but support functions slow—so staying current keeps you near the front of the post-shutdown queue (OPM; HHS contingency plan).
The Bottom Line: Turning Shutdown Chaos into Long-Term Strength

If this government shutdown healthcare saga has taught us anything, it’s that resilience isn’t built during calm times — it’s forged in the middle of a slowdown. The payment delays were frustrating, yes, but they also revealed where many practices are vulnerable and how much smoother operations can be with better preparation.
You now understand what happens when CMS activity slows to half-speed, why Medicare claim processing delays ripple through every corner of the healthcare system, and how to safeguard your cash flow when oversight staff are temporarily furloughed.
The good news? These aren’t one-time lessons.
If you’ve spent the past few weeks tightening your claim workflows, communicating openly with staff, and tracking your accounts like a hawk, you’re already miles ahead. Use that momentum to reinforce your healthcare financial planning during shutdown — even when the government is running normally.
Set aside reserves. Automate your clean-claim checks. Train your staff to understand the difference between essential and nonessential operations so they can adapt quickly next time. Keep those CMS and MAC newsletters bookmarked.
Most importantly, remember that you can’t control Washington, but you can control how prepared your practice is to handle its ripple effects. Each delay, each backlog, and each late payment is a reminder to stay proactive, not reactive.
So, when the next Federal Government Shutdown impacts Healthcare, and it likely will, you won’t just be waiting for the system to catch up. You’ll be ready, steady, and already a step ahead of the curve.
Because surviving a shutdown isn’t just about getting through it, it’s about coming out smarter, stronger, and sharper than before.
Jennifer Blevens-Smith, founder of Integral Clinic Solutions, helping practices master the art of balancing patient satisfaction with quality care.
This article is for informational and operational planning purposes only and isn’t financial, legal, tax, or billing advice. Policies and agency operations can change; always verify details with official CMS/HHS guidance and your MAC, legal counsel, or compliance team. We do not receive compensation from government agencies or payers referenced. No patient-level decisions should be made based solely on this content.
