Healthcare Q4 Planning Guide for Busy Clinics
The fourth quarter hits like a freight train every year—and without solid Q4 planning, most healthcare practices get caught off guard. Strategic preparation means thriving during the most profitable quarter, not just surviving the chaos. Smart practice managers know this season can make or break their annual revenue goals.
Key Takeaways
- Q4 is the busiest and most profitable quarter for healthcare—planning early is crucial.
- Patients rush in due to met deductibles; practices must prepare for volume spikes.
- Staffing, scheduling, and insurance verification systems need proactive adjustments.
- AR cleanup in Q4 directly boosts Q1 cash flow.
- Compliance changes and cybersecurity threats spike during Q4.
- Backup systems and technology upgrades should be finalized before January 1st.
- Smart Q4 planning sets a strong launchpad for January success.
Other businesses wind down for the holidays. Healthcare practices see their biggest surge. Patients flood the phones, staff scramble to handle demand, and revenue opportunities multiply or disappear based on preparation. Well-prepared practices often outperform competitors by 30-40% during this period.
Table of Contents
Why Q4 Turns Into Chaos for Healthcare Practices

Planning for the Year-End Deductible Surge
Picture this: It’s November, and Sarah realizes she’s spent $4,800 toward her $5,000 deductible this year. That knee surgery she’s been putting off suddenly looks affordable. She’s not alone. Millions of patients have this same realization at once.
Patients who have met their deductibles become appointment-seeking missiles during Q4. They’ve prepaid for healthcare through deductible payments. Now they want maximum value before January 1st resets everything to zero. This creates a surge that can overwhelm unprepared practices.
The psychology is simple. Patients treat remaining deductibles like use-it-or-lose-it vacation days. They schedule procedures, consultations, and treatments they’ve delayed all year. Specialty practices like orthopedics and podiatry see this most dramatically. Patients can postpone non-emergency treatments until it’s financially smart.
Managing Patient Volume During Sick Season
Q4 brings the annual sick season to your doorstep. Kids return to classrooms and spread everything from colds to serious infections. Parents catch bugs from children, creating ripple effects through families and workplaces.
Primary care practices and internal medicine clinics get hit twice. They handle the deductible rush crowd and genuinely sick patients who can’t wait. This combination pushes patient volumes 40-60% higher than typical quarters.
The timing creates maximum challenge. Just when practices need peak efficiency, they’re dealing with peak complexity. Sick patients need immediate attention. Deductible-motivated patients want multiple procedures scheduled before year-end.
Smart Q4 Planning Strategies Busy Practices Use
Staff Scheduling Tactics That Support Q4 Planning
Successful practices don’t hope their current staff can handle Q4 volume. They plan staffing changes months ahead. This means having conversations about schedule changes, overtime availability, and temporary staff before the rush hits.
Adding practice hours during Q4 isn’t about burning out your team. It’s about smart capacity expansion. Some practices extend evening hours or add Saturday appointments for Q4. Others cross-train staff to handle multiple roles during peak periods.
The key is changing staff schedules strategically, not just adding more work to existing schedules. Maybe your front desk coordinator works four 10-hour days instead of five 8-hour days. This provides coverage during peak calling hours while maintaining work-life balance. providing coverage during peak calling hours while maintaining work-life balance.
| Staffing Strategy | Implementation Timeline | Expected Impact |
| Extended evening hours | 6 weeks before Q4 | 20-30% capacity increase |
| Cross-training programs | 8 weeks before Q4 | Improved flexibility |
| Temporary staff hiring | 4-6 weeks before Q4 | Direct volume management |
| Schedule optimization | Ongoing through Q3 | Maximum efficiency |
Use Year-End Volume to Build Revenue Momentum
Most practice owners miss this: Q4 revenue collection isn’t just about this quarter. It’s about creating momentum that carries through Q1’s deductible season. Every dollar you collect in Q4 becomes fuel for surviving the lean months when patients’ deductibles reset.
Think of Q4 as your practice’s version of squirrels gathering nuts for winter. The more you collect during high-volume months, the better positioned you’ll be when January hits and patients become cost-conscious again.
Using Q4 demand requires balancing immediate revenue with long-term patient relationships. You can’t just grab cash during busy periods. You need to deliver excellent service that keeps patients coming back when their finances improve.
Insurance Verification Tips for a Stress-Free Year-End
Avoiding Over-Collection Pitfalls in Q4
Most practices celebrate when patients pay upfront deposits. But Q4 creates a dangerous trap. Insurance verification becomes critical when patients are close to meeting deductibles or have hit out-of-pocket maximums. Get this wrong, and you’ll drown in patient credits and refund requests.
Here’s what catches practices off guard: Maria schedules her procedure in November. Your front desk collects an $800 deposit based on her unmet deductible. They don’t realize Maria only has $200 left on her deductible. When insurance processes the claim, you’ve overcollected by $600 and owe her money.
Checking patient deductible status isn’t just good practice. It’s financial survival. Your front office staff need real-time access to patients’ current benefit use. This means calling insurance companies, using online portals, or investing in verification software that provides current data.
The stakes get higher with out-of-pocket maximum verification. Patients who’ve reached their annual limits shouldn’t pay copays or coinsurance. Yet practices routinely collect these payments out of habit, creating admin nightmares and unhappy patients.
Related: How to Navigate Deductible Season Without Financial Stress
Systems That Simplify Insurance Verification
Create a systematic approach to flagging deductible resets in your practice system. When you verify benefits for Q4 patients, add notes showing their deductible resets on January 1st. This simple step prevents major headaches in the new year.
Insurance plan changes happen often at year-end when employers modify their offerings. That patient who’s been coming all year might show up in January with completely different coverage. Your deductible reset flags serve double duty by prompting staff to reverify coverage for new-year appointments.
Consider implementing this verification workflow:
| Verification Step | Timing | Staff Responsible | Documentation Required |
| Initial benefit check | At scheduling | Registration | Current deductible status |
| Pre-service verification | 48 hours before | Front office | Remaining deductible amount |
| Day-of confirmation | Check-in | Registration | Any changes since last visit |
| Post-service reconciliation | Within 24 hours | Billing | Actual vs. collected amounts |
Holiday Staffing Solutions That Actually Work
Solving the Holiday Staffing Puzzle
Holiday scheduling in healthcare requires chess-master thinking. Halloween falls on Friday this year. Thanksgiving creates a four-day weekend. Christmas vacation requests start before October ends. Meanwhile, you’re seeing peak patient volume.
The secret isn’t denying all vacation requests. It’s creating fair time-off policies that everyone understands before requests start flying. Set clear criteria: seniority, rotation systems, or first-come-first-served. Pick a system, communicate it early, and stick to it.
Provider vacation coordination gets even trickier. If Dr. Smith takes Thanksgiving week off, you can’t approve Dr. Jones’s Christmas week request if they’re your only two physicians. Map out provider availability before patients start booking Q4 appointments.
Prevent Q4 Scheduling Disasters With Smart Systems
Nothing frustrates patients more than showing up for appointments with providers who are on vacation. Updating provider schedules immediately when time-off gets approved prevents these embarrassing mistakes. Your scheduling system should show real availability, not wishful thinking.
Try blocked scheduling for holiday periods. Instead of leaving slots open for providers who might be unavailable, block those times completely. This forces realistic scheduling and prevents overbooking disasters.
Some practices create holiday schedule templates that automatically account for reduced staffing. These templates help you avoid scheduling 40 patients when your capacity is only 25.
AR Management That Saves Your Year-End Cash Flow
Last-Chance AR Cleanup Before Year-End

Working your AR hard during Q4 isn’t just good bookkeeping. It’s smart financial planning. Every claim you resolve in Q4 means money in the bank during Q1’s deductible drought. This is your chance to clean house and collect on delayed payments before they become write-offs.
Getting chart notes completed becomes critical during this period. Providers often fall behind on documentation during busy times. But incomplete charts prevent claim submission. Create systems that ensure notes get finished within 24-48 hours of patient visits.
The math works like this: Claims submitted in December for services from throughout the year often get paid in January or February. This happens right when new deductibles are slowing down patient payments. It creates a financial bridge that smooths out the typical Q1 cash flow dip.
Forecasting Q4 and January Cash Flow Needs
Planning cash flow for December through February requires understanding seasonal payment patterns. Patients spend heavily on holidays. Insurance companies process claims slower during year-end. Collection rates typically drop 15-25% during this period.
Smart practices build financial cushions during Q4 to weather these predictable storms. This isn’t about hoarding money. It’s about planning that keeps your practice stable when revenue becomes unpredictable.
Compliance Changes Coming in Q4: Are You Ready?
Regulatory Reset: What Changes January 1st
CMS policy changes don’t trickle in slowly. They hit like an avalanche every January 1st. While you’re managing Q4 chaos, federal agencies are finalizing regulations that could completely change how you operate next year. Ignoring these updates isn’t just risky. It’s expensive.
HIPAA updates often take effect at year-end with minimal fanfare but maximum impact. These changes might affect how you handle patient communications, store electronic records, or process insurance claims. Practices that stay ahead avoid costly violations and operational disruptions.
Your compliance checklist should include regular visits to OIG, HHS, and CMS websites. Don’t wait for industry newsletters to inform you about changes. Go directly to the source. Set calendar reminders for the first Tuesday of each month during Q4 to check for new announcements.
Insurance guideline changes can be equally disruptive but often get overlooked. Insurance companies regularly update coverage policies, prior authorization requirements, and payment schedules effective January 1st. What your practice could bill freely in December might require extensive documentation in January.
Build a Year-End Compliance Tracker
Create a systematic approach to tracking changes rather than hoping you’ll catch important updates by accident. Assign specific team members to monitor different agencies and payers. This spreads the workload and ensures nothing falls through the cracks.
Cybersecurity Threats Surge in Q4—Here’s How to Prepare
Q4 Cyber Threats: Why Healthcare Is Targeted
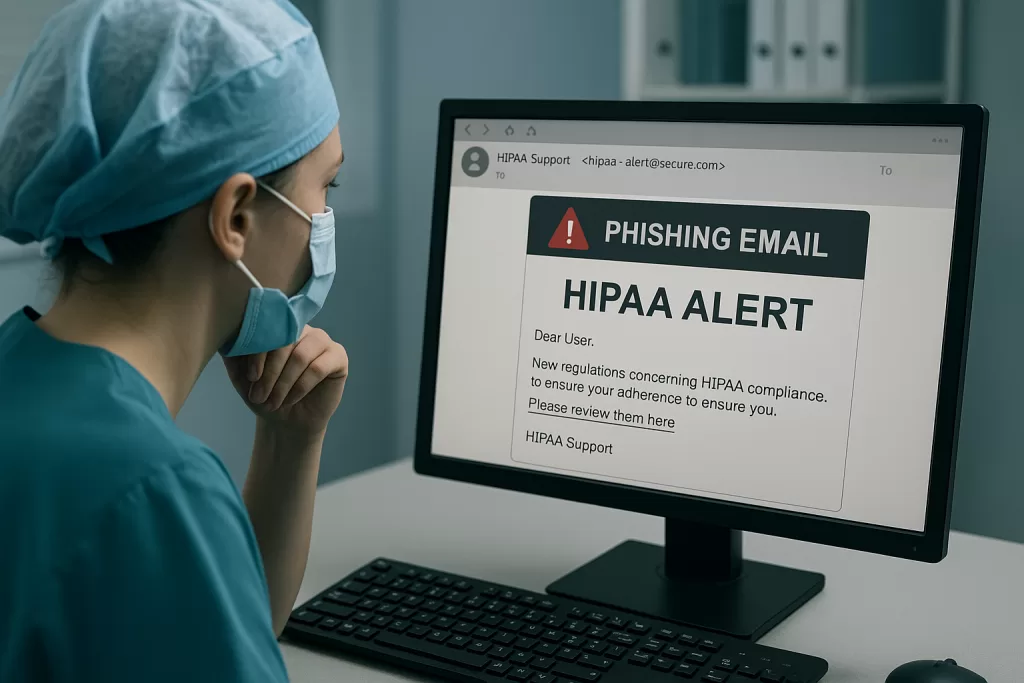
Cybersecurity breaches spike during Q4. Healthcare practices make attractive targets. Cybercriminals exploit holiday chaos, knowing busy staff are more likely to click suspicious links or fall for sophisticated scams.
Healthcare phishing scams often look like compliance updates or urgent policy changes. These emails create fake panic, pushing people to click malicious links or download infected files. When your staff are already stressed about real compliance deadlines, fake urgency becomes incredibly effective.
The money behind targeting healthcare practices is substantial. Medical records sell for much more than credit card information on illegal markets. A single successful breach can compromise thousands of patient records and result in devastating HIPAA violations.
Holiday-related scams targeting patients also create indirect risks for your practice. When patients’ personal information gets compromised through retail breaches or social engineering, it can lead to insurance fraud that impacts your claims processing and patient accounts.
Make Q4 Cybersecurity a Team Priority
Security awareness training becomes essential before Q4 gets intense. Your staff need fresh reminders about identifying suspicious emails, especially when dealing with increased communication and stress levels. Tired, overwhelmed employees make more mistakes.
Work with your IT security specialist to add extra safeguards during peak periods. This might include enhanced email filtering, more frequent security updates, or temporary restrictions on certain file downloads during high-risk periods.
Build a “when in doubt, don’t click” culture where staff feel comfortable asking questions about suspicious communications rather than making quick decisions that could compromise your entire network.
End-of-Year Service Expansions That Make Sense
Year-End Is Backup Season—Are You Ready?
EMR backup procedures become extra important as you approach year-end. You’re not just protecting against system failures. You’re creating clean break points between fiscal years that make future data retrieval much easier.
Separate billing software backup often gets forgotten because it’s not part of the main EMR system. However, this software contains crucial financial data you’ll need for tax prep, audit responses, and year-end reporting. Losing this information creates compliance nightmares and financial reporting disasters.
Electronic document storage goes beyond medical records to include contracts, policies, correspondence, and financial documents. Create a complete backup strategy that covers every system containing practice-critical information.
Working With IT to Prepare for System Failures
Your IT backup strategy should address both routine protection and year-end organization. This means not just copying data, but organizing it in ways that support efficient retrieval and year-end reporting requirements.
Test your backup systems before you need them. Many practices discover their backup procedures don’t work only when trying to recover from a disaster. Schedule test restorations during slower periods to identify and fix problems before Q4 chaos begins.
How to Set Strategic Benchmarks for Next Year’s Success
Financial Metrics That Shape Next Year’s Goals
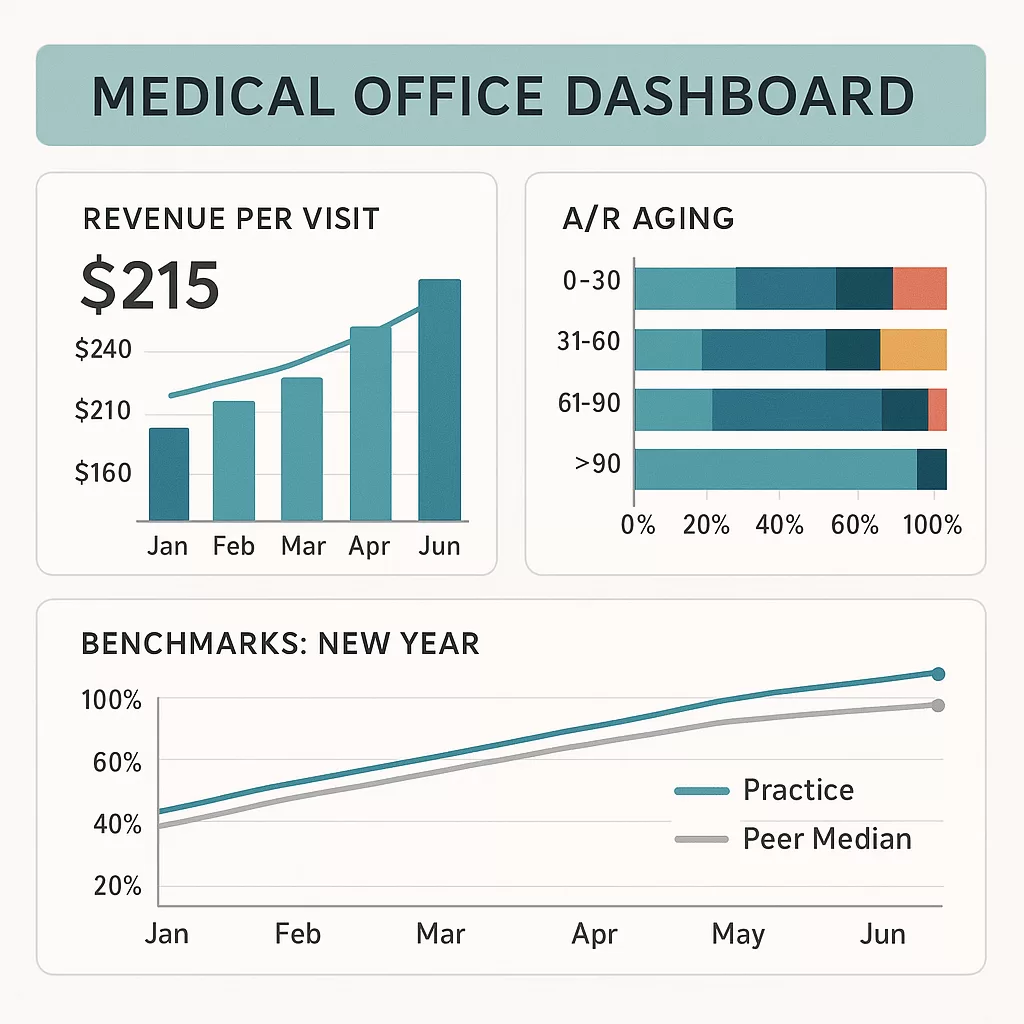
Setting benchmarks for next year during Q4 isn’t about picking random numbers. It’s about creating measurable goals based on realistic performance data. The most successful practices use Q4 as their strategic planning season, analyzing current year performance to set achievable yet ambitious targets.
Financial performance benchmarks should reflect both your practice’s growth potential and market realities. Look at revenue per patient visit, collection rates, and accounts receivable aging to establish baseline metrics. Then factor in planned changes like new services, additional providers, or technology investments that could impact these numbers.
Staffing efficiency measurements become crucial when planning for growth. Calculate your current patient-to-staff ratios, revenue per employee, and overtime costs. These metrics help determine whether you need additional team members or if process improvements could handle increased volume more efficiently.
Create benchmarks that motivate rather than intimidate. Set targets that require effort but remain achievable with focused execution. Unrealistic goals demoralize teams. Easy targets waste growth opportunities.
Planning Investments Before Year-End Deadlines
Large equipment purchases require months of planning, especially when they impact your physical space or require staff training. Q4 provides the perfect opportunity to research options, compare vendors, and create implementation timelines for major acquisitions.
Technology adoption planning has become increasingly important as healthcare digitization accelerates. Whether you’re considering AI-powered scheduling systems, telemedicine platforms, or enhanced EMR capabilities, Q4 gives you time to evaluate options without rushing decisions.
Budget planning for growth investments requires balancing current cash flow with future revenue potential. Map out payment schedules for major purchases against projected revenue increases to ensure you maintain healthy cash flow throughout the investment period.al. Map out payment schedules for major purchases against projected revenue increases to ensure you maintain healthy cash flow throughout the investment period.
Related: Budget Planning for Medical Practices: 10 Must-Know Strategies for Financial Stability
| Investment Type | Planning Timeline | Key Considerations | ROI Timeframe |
| Medical equipment | 6-12 months | Space, training, financing | 12-24 months |
| Technology upgrades | 3-6 months | Intergration, staff adoption | Integration, staff adoption |
| Facility expansion | 12-18 months | Permits, construction, disruption | 18-36 months |
| New service lines | 6-9 months | Certification, marketing, equipment | 9-24 months |
What Service Expansions Make Sense for Your Practice?
Exploring Cash-Pay Services for Year-End Stability
Service expansion planning often focuses on insurance-reimbursed procedures, but cash-pay services provide stable revenue streams that aren’t subject to deductible changes. Aesthetic services like Botox injections, wellness programs, or concierge medicine models create predictable income that smooths out seasonal variations.
Cash-only services offer beautiful simplicity. No insurance verification, no claim submissions, no denial management. Just direct patient payment for services rendered. This becomes particularly appealing when dealing with traditional healthcare billing complexity.
Market research for new services should include both patient demand analysis and competitive landscape evaluation. Survey your existing patients about services they’d value. Research what similar practices in your area are offering successfully.
Tech Upgrades That Strengthen Practice Efficiency
AI adoption in healthcare has moved from experimental to essential in many specialties. Whether it’s automated appointment scheduling, clinical decision support, or administrative task automation, AI tools can significantly improve practice efficiency and patient satisfaction.
Successful technology implementation lies in choosing solutions that integrate smoothly with existing systems rather than creating additional complexity. Look for platforms that enhance current workflows rather than forcing complete process overhauls.
Research and evaluation timelines for new technology should allow for thorough testing and staff training. Rushing technology adoption during busy periods often leads to implementation failures and staff frustration.
Beat the Post-Holiday Slump with Smart Year-End Moves
Don’t Let Post-Q4 Slump Kill Your Momentum
The holiday hangover effect kills practice productivity every January. Staff return from vacation feeling sluggish. Patients delay scheduling due to new deductibles. Everyone moves in slow motion. Smart practices flip this script completely.
Building excitement for the new year starts with how you frame the transition. Instead of dreading deductible season, position January as an opportunity to implement improvements, launch new services, or achieve ambitious goals. Your leadership attitude sets the tone for the entire practice.
Staff motivation strategies during the holiday transition require balancing recognition for Q4 achievements with enthusiasm for upcoming opportunities. Celebrate successful quarters while building anticipation for new initiatives and improvements.
What is Q4 planning in healthcare?
Q4 planning in healthcare refers to the strategic preparation that medical practices undertake during the final quarter of the year. It includes managing deductible-driven patient surges, optimizing staff schedules, improving billing processes, and preparing for regulatory or insurance changes that typically begin on January 1st.
Why is Q4 so critical for medical practices?
Q4 is often the busiest—and most profitable—time of year for healthcare practices. Patients rush to use up benefits before deductibles reset, while flu season and holiday scheduling challenges compound the chaos. Practices that plan well can see a 30–40% revenue bump.
How can I prepare my staff for the Q4 rush?
Start early. Review time-off policies, cross-train team members, consider extending office hours, and clearly communicate expectations. Proactive staffing adjustments help prevent burnout and missed revenue opportunities during peak patient volume.
What’s the best way to verify insurance benefits in Q4?
Double-check deductible and out-of-pocket statuses before collecting payments. Use online portals or call insurance companies directly to confirm benefits. Set up workflows that flag year-end resets so your staff avoids overcharging or undercharging patients.
How should I handle AR management before the year ends?
Focus on cleaning up aging claims, ensuring chart notes are complete, and submitting outstanding charges before December 31st. This gives you a financial cushion to navigate Q1’s usual dip in patient payments due to fresh deductibles.
Are there any compliance updates I should watch for during Q4?
Yes—Q4 is when CMS, HIPAA, and commercial payers announce policy changes that take effect January 1st. Assign team members to monitor updates from OIG, HHS, and key insurers weekly so you’re not caught off guard.
Why are cybersecurity risks higher in Q4?
Cyberattacks often spike during the holiday season when staff are distracted or working under pressure. Scams disguised as compliance alerts or vendor emails are common. Make cybersecurity training and email vigilance part of your Q4 planning.
What backup strategies should be in place before year-end?
Ensure all systems—EMR, billing, financial documents—are backed up to secure, offsite storage. Test your restore processes. Partner with your IT team to review security protocols and prepare for high-risk periods.
Can Q4 planning help my practice start January stronger?
Absolutely. Smart Q4 planning not only boosts year-end revenue but also sets the tone for Q1. Address staffing, cash flow, service expansion, and compliance during Q4 so your team hits the ground running after the holidays.
January 1st: Launch the Year With Confidence

Hitting the ground running on January 1st requires preparation during Q4, not wishful thinking over winter break. Create specific action plans for the first week of January that give your team clear directions and immediate wins.
Introducing new initiatives at year-end provides natural timing for implementation. Whether it’s new scheduling software, updated policies, or enhanced patient communication systems, January 1st offers a psychological fresh start that makes change adoption easier.
Momentum building activities might include staff training on new procedures, patient communication about expanded services, or internal process improvements that create immediate efficiency gains. The goal is making January feel like a launch rather than a recovery.
Q4 preparation in healthcare isn’t optional. It’s the difference between practices that thrive and those that merely survive. The strategies outlined here transform traditional year-end chaos into organized opportunity.
Start implementing these changes immediately. Don’t wait for the perfect moment or complete information. Preparing for Q4 in healthcare requires action, adaptation, and the courage to make decisions with imperfect information.
The practices that dominate their markets aren’t necessarily the ones with the best locations or most prestigious reputations. They’re the ones that prepare systematically and execute consistently. Make this Q4 the quarter that sets your practice apart from the competition.
Written by Jennifer Blevens-Smith, founder of Integral Clinic Solutions and host of the YouTube channel “Navigating the Business of Medicine.” Jennifer helps private practices strengthen compliance, streamline vendor relationships, and protect their bottom line from costly mistakes.
